
A RARE CASE OF DYSPNEA
Petre Olvis 1![]()
![]() ,
Tashi Bani Irma 1, Hasani Jola 1, Shestani Justi 1, Bala Silvana 1, Hafizi
Hasan 1
,
Tashi Bani Irma 1, Hasani Jola 1, Shestani Justi 1, Bala Silvana 1, Hafizi
Hasan 1
1 Pulmonology Department, “ShefqetNdroqi”
University Hospital, Albania
|
|
ABSTRACT |
||
|
Idiopathic dilatation of the pulmonary artery defines the presence of a benign enlargement of the pulmonary trunk with or without the involvement of the rest of the arterial tree in the absence of a detectable cardiac or arterial systemic disorder. An IDPA patient’s symptoms and physical examination are not significant in diagnosis confirmation. Imaging techniques such as contrast-enhanced computed tomography, right heart catheterization, and angiocardiogram constitute the foundation of IDPA diagnosis. But an extended observation period is also necessary to exclude other possible dilatation explanation. Our patient, a forty-six-year-old female, was admitted to the Pulmonology clinic of “ShefqetNdroqi” University Hospital with dyspnea, dry cough, vertigo, and fatigue for several months before admission. The patient's contrast-enhanced Computed Tomography revealed a dilatation of the pulmonary trunk. The dilatation of the pulmonary trunk was confirmed with the Cardiac CT, and other abnormalities were excluded. |
|||
|
Received 09 December 2022 Accepted 10 January 2023 Published 31 January 2023 Corresponding Author Petre Olvis,
olvispetre@yahoo.com DOI 10.29121/granthaalayah.v11.i1.2023.4931 Funding: This research
received no specific grant from any funding agency in the public, commercial,
or not-for-profit sectors. Copyright: © 2023 The
Author(s). This work is licensed under a Creative Commons
Attribution 4.0 International License. With the
license CC-BY, authors retain the copyright, allowing anyone to download,
reuse, re-print, modify, distribute, and/or copy their contribution. The work
must be properly attributed to its author.
|
|||
|
Keywords: IDPA, Idiopathic Dilatation of The
Pulmonary Artery, Contrast-Enhanced CT |
|||
1. INTRODUCTION
Idiopathic dilatation of the pulmonary artery (IDPA) defines the presence of a benign enlargement of the pulmonary trunk with or without the involvement of the rest of the arterial tree in the absence of a detectable cardiac or arterial systemic disorder. Greene et al. (1949) The diagnosis of idiopathic dilatation of the pulmonary artery relies on specific criteria, which were first proposed by Greene et al. (1949). and later improved upon by Deshmukh et al. (1960). The latter addition included the evaluation of the right ventricle and pulmonary artery pressure to exclude pulmonary hypertension as a cause of this enlargement.
Etiologically speaking, IDPA is related to a congenital arterial wall weakness, which leads to cystic degeneration of the pars media. Balboni and Lopresti (1961) This is the most accepted theory related to the histopathology of IDPA, but more concrete evidence is necessary.
2. CASE REPORT
Our forty-six-year-old female patient was admitted to the Pulmonology clinic of “ShefqetNdroqi” University Hospital on May 11th, 2017. She complained of exertional dyspnea, dry cough, vertigo, and fatigue for several months before admission. Physical examination was unremarkable. The arterial blood gasses examination revealed a level of oxygen saturation of 94%, with hypocapnia (paCO2 32.3 mmHg) and normal oxygen arterial pressure (paO2 65.9 mmHg).
The
patient's contrast-enhanced Computed Tomography revealed a diameter of the
pulmonary trunk (44 mm), right pulmonary artery (33 mm), and left pulmonary
artery (25 mm). Figure 1 No significant abnormality
of the lung parenchyma was noted. In the abdominal cavity, the CT revealed
hepatosplenomegaly Figure 2 and a lesion in the eighth
hepatic segment (hemangioma). The portal vein diameter was estimated to be 16
mm, the spleen vein diameter 15 mm, and the superior mesenteric vein 11 mm.
Figure 1

|
Figure 1 Axial View of the Dilated Pulmonary Trunk from the Contrast-Enhanced CT |
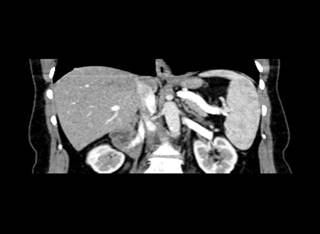
Figure 2
|
Figure 2 Coronal View of the Hepatosplenomegaly from the Contrast-Enhanced CT |
Trans-esophageal
echocardiography revealed an interatrial septal aneurysm with a minimal left to
right shunt, without contrast displacement from the right side to the left
during the Valsalva maneuver. This examination had no detectable pulmonary
artery dilation or significant transvalvular gradient or regurgitation.
Because
of the inconsistent findings in these imaging examinations, further
investigation was required, and the patient underwent cardiac computed
tomography examination and right heart catheterization. The dilatation of the
pulmonary trunk was confirmed with the Cardiac CT Figure 3 and Figure 4, and its diameter was
estimated to be 41 mm. In contrast, the left and right pulmonary arteries
remained intact, with a diameter of 21 and 26 mm, respectively.
Figure 3

|
Figure 3 Image from the Cardiac CT (Frontal) |
Figure 4

|
Figure 4 Image from the Cardiac CT (Lateral) |
Right
heart catheterization denoted a wedge pressure of 15/7 mmHg, a pulmonary artery
pressure of 21/9 mmHg, and a pulmonary trunk pressure of 23/11 mmHg.
3. DISCUSSIONS
IDPA
symptoms include dyspnea on exertion, tachycardia, exhaustion, and chest pain. Malviya et al. (2017) These symptoms are not significant in diagnosis
confirmation, because they are mainly related to the disease’s complications
from compression of surrounding tissues leading to massive extension,
thrombosis, or even rupture. Taussig (1947), Copkiran et al. (2014), Puri et al. (2011). Myocardial infarction has
been described in cases of huge dilatation of pulmonary artery related to the
compression of coronary arteries and sudden cardiac arrest may also happen. Jurado-Román et al. (2013), Andrews et al. (1993). But in most cases, IDPA is
an incidentaloma, and patients either exhibit mild non-specific symptoms or
have no symptoms. This often leads to underdiagnosis and misdiagnosis of IDPA. Zhao and Cheng (1992).
Physical
examination also does not play a significant role in the diagnostic process. In
most cases, physical examination is interpreted as inconclusive. Van Buchem et al. (1955)Experts, however, recommend
acknowledging IDPA as part of the differential in a patient with minimal
symptoms and systolic, diastolic, or both cardiac murmurs. Kaplan et al. (1953).
Imaging
techniques such as cardiac contrast-enhanced computed tomography constitute the
foundation of IDPA diagnosis. It evaluates the artery enlargement's exact
location and morphological characteristics and provides information about
possible concomitant abnormalities. Nguyen et al. (2007)
The
diagnosis can be confirmed only by excluding other cardiovascular or systemic
causes of the dilated pulmonary artery. This information can be obtained
through additional imaging techniques such as heart catheterization and cardiac
magnetic resonance imaging. Futagami et al. (1987), Ugolini et al. (1999).
Even
though almost ten decades have passed since IDPA was first described as an anomaly
Wessler and Jaches (1923), it remains a real challenge
for clinicians because of its tendency to imitate cardiac disorders and the
non-specificity of its symptoms. It represents an exclusion diagnosis and
requires long observation periods as some underlying pathologies come into view
as the disease progresses. Ring et al. proposed including the observation
period in the diagnostic criteria. Ring, and Marshall (2002).
4. CONCLUSIONS AND RECOMMENDATIONS
Patients with IDPA have a wide range of clinical presentations. The symptoms might range from being unintentionally discovered to life-threatening manifestations typically connected to serious illness complications from the extension of the dilatation.
IDPA is a diagnosis by exclusion. It necessitates a good understanding of the diagnostic criteria and sharp observational skills from a multidisciplinary team, which includes pulmonologists, radiologists, and cardiologists.
Although imagery examination, such as contrast-enhanced cardiac CT or other advanced imaging techniques may give a detailed view of the structures involved in this anomaly, an extended observation period may be necessary to rule out any secondary causes of the dilatation.
CONFLICT OF INTERESTS
None.
ACKNOWLEDGMENTS
None.
REFERENCES
Andrews,
R., Colloby, P., and Hubner, P. J. (1993). Pulmonary Artery Dissection
In A Patient With Idiopathic Dilatation of The Pulmonary Artery: A Rare Cause of
Sudden Cardiac Death. British Heart Journal, 69(3), 268-269. https://doi.org/10.1136/hrt.69.3.268.
Balboni,
F. A., and Lopresti, J. (1961). Congenital Idiopathic Dilatation of The
Pulmonary Artery in Children. A Report of Seven Cases [Bulletin]. Bulletin. Roslyn,
N. Y. St. Francis Hospital and Sanatorium for Cardiac Children, 17, 1-21.[5] Van
Buchem, F. S. P., Nieveen, J., Marring, W., and Van Der Slikke, L. B. (1955). Idiopathic
Dilatation of The Pulmonary Artery. Diseases of the Chest, 28(3), 326-336. https://doi.org/10.1378/chest.28.3.326.
Copkiran,
O., Akcay, S., Ozben, C., Ozdemir, I., and Tarhan, S. (2014). Extreme Pulmonary
Artery Aneurysm With Thrombosis. Medical Science and Discovery, 1(4), 118-120. https://doi.org/10.17546/msd.68822.
Deshmukh,
M., Guvenc, S., Bentivoglio, L., and Goldberg, H. (1960). Idiopathic Dilatation
of the Pulmonary Artery. Circulation, 21(5), 710-716. https://doi.org/10.1161/01.cir.21.5.710.
Futagami, Y., Yada, T., Konishi, T., Iwata, J., Hamada, M., and Nakano, T. (1987). Idiopathic Dilatation of the Pulmonary Artery: A Case Report and Review of 59 Cases in Japan. Mieigaku, 31, 425-432.
Greene, D. G., Baldwin, E. D., Baldwin, J. S., Himmelstein, A., Roh,
C. E., and Cournand, A. (1949). Pure Congenital Pulmonary Stenosis and
Idiopathic Congenital Dilatation Of The Pulmonary Artery. American Journal Of Medicine,
6(1), 24-40. https://doi.org/10.1016/0002-9343(49)90004-2.
Jurado-Román, A., Hernández-Hernández, F., Ruíz-Cano,
M. J., Velázquez-Martín, M. T., Medina, J. M., Pérez-López, I., Barrios-Garrido-Lestache,
E., Montero-Cabezas, J. M., and Escribano-Subías, P. (2013). Compression
of the Left Main Coronary Artery By A Giant Pulmonary Artery Aneurysm. Circulation,
127(12), 1340-1341.
https://doi.org/10.1161/CIRCULATIONAHA.112.152199.
Kaplan, B. M., Schlichter, J. G., Graham, G., and Miller, G. (1953). Idiopathic Congenital Dilatation of the Pulmonary Artery. Journal of Laboratory and Clinical Medicine, 41(5), 697-707.
Malviya, A., Jha, P. K., Kalita, J. P., Saikia, M. K., and Mishra, A. (2017). Idiopathic Dilatation of Pulmonary Artery: A Review. Indian Heart Journal, 69(1), 119-124. https://doi.org/10.1016/j.ihj.2016.07.009.
Nguyen,
E. T., Silva, C. I., Seely, J. M., Chong, S., Lee, K. S., and Müller, N. L.
(2007). Pulmonary Artery Aneurysms and Pseudoaneurysms in Adults: Findings
at CT and Radiography. AJR. American Journal of Roentgenology, 188(2), W126-W134. https://doi.org/10.2214/AJR.05.1652.
Puri,
D., Kaur, H. P., Brar, R., Singh, K. P., Sahoo, M., and Mahant, T. S. (2011).
Ruptured Pulmonary Artery Aneurysm: A Surgical Emergency. Asian Cardiovascular and
Thoracic Annals, 19(6), 436-439. https://doi.org/10.1177/0218492311421443.
Ring, N. J., and Marshall, A. J. (2002). Idiopathic Dilatation of the Pulmonary Artery, the British Journal of Radiology 75(894), 532-535. https://doi.org/10.1259/bjr.75.894.750532.
Taussig, H. B. (1947). Congenital Malformations of the Heart. In Congenital Malformations of the Heart, 654-654.
Ugolini, P., Mousseaux, E., Sadou, Y., Sidi, D., Mercier, L. A., Paquet, E., and Gaux, J. C. (1999). Idiopathic Dilatation of the Pulmonary Artery: Report of Four Cases. Magnetic Resonance Imaging, 17(6), 933-937. https://doi.org/10.1016/s0730-725x(99)00013-2.
Van
Buchem, F. S. P., Nieveen, J., Marring, W., and Van Der Slikke, L. B. (1955).
Idiopathic Dilatation of the Pulmonary Artery. Diseases of the Chest, 28(3),
326-336. https://doi.org/10.1378/chest.28.3.326.
Wessler, H., and Jaches, L., (1923). The Southworth Company, and Troy, N. J./New York. Clinical Roentgenology of Disease of The Chest. 26. Ring. British Journal of Radiology. AJ (2002).
Zhao, Y. J., and Cheng, X. S. (1992). An Analysis of 21 Cases of Idiopathic Dilatation of The Pulmonary Artery. Zhonghuaneikezazhi, 31(1), 24-25.
 This work is licensed under a: Creative Commons Attribution 4.0 International License
This work is licensed under a: Creative Commons Attribution 4.0 International License
© Granthaalayah 2014-2023. All Rights Reserved.