ShodhKosh: Journal of Visual and Performing ArtsISSN (Online): 2582-7472
|
|
Sound, Technology, and Healing: Exploring Music Therapy in Healthcare
Nisha Wankhade 1![]() , Sharmishtha K. Garud 2
, Sharmishtha K. Garud 2![]() , Kiran
Bibhishan Naikwadi 3
, Kiran
Bibhishan Naikwadi 3![]() , Dr.
E. Rajesh 4
, Dr.
E. Rajesh 4![]() , Ashifa
Kariveliparambil 5
, Ashifa
Kariveliparambil 5![]() , Dr.
Vijay Suresh Karwande 6
, Dr.
Vijay Suresh Karwande 6![]()
1 Department
of Information Technology, Yeshwantrao Chavan College
of Engineering, Nagpur, India
2 Department
of Community Medicine, Krishna Institute of Medical Sciences, Krishna Vishwa
Vidyapeeth (Deemed to be University), Taluka-Karad, Dist-Satara,
Pin-415 539, Maharashtra, India
3 Department of Engineering Sciences and Allied Engineering, Bharati
Vidyapeeth's College of Engineering for Women, Dhankawadi,
Pune, Maharashtra, India
4 Department of Oral and Maxillofacial Pathology and Oral Microbiology,
Sree Balaji Dental College and Hospital, Chennai, Tamil Nadu, India
5 Faculty of Health Sciences, Istanbul Gelisim
University, Turkey
6 Assistant Professor, Department of Computer Engineering, Sandip
Institute of Technology and Research Centre, Nashik, India
|
|
ABSTRACT |
||
|
The growing
popularity of music therapy as a complementary treatment option in the
contemporary healthcare system is associated with the capacity of this method
to promote emotional, psychological, and physiological health. By combining
the sound-based therapeutic practice with the new digital technology, the
application has opened new possibilities of making the music therapy
interventions more effective and more accessible. This paper analyzes the
interface of sound, technology, and healing through the aspects of music
therapy within the medical facility context and the possibilities of
technology-based systems of therapeutic assistants. The paper involves itself
in the history and theories of music therapy, and highlights the
psychological and neurological processes involved in the human health in the
sound process. An in-depth survey of the literature available points at the
clinical usability of music therapy in mental health care, neurological
rehabilitation, pain control, and patient care. The study is also exploring
the potential of the emerging technologies, such as digital audio processing,
wearable health sensors, artificial intelligence, mobile health applications,
and immersive virtual environments, in assisting personalized music therapy
intervention. The technologies allow creating adaptive therapeutic systems
that react on patient physiological indications and emotional conditions in
real-time. On the basis of this analysis, the paper will present a
technology-based model of music therapy aimed at incorporating patient
monitoring, generating therapeutic music, interactive feedback systems, and
connecting with healthcare systems. The framework that is offered to be
implemented will contribute to better patient interactions, increased therapy
customization, and the possibility to evaluate the effectiveness of therapy
using the data. In addition, the paper addresses the measures of evaluation
of clinical ecoefficiency, usability, and ethical evaluation of
technology-based music therapeutic systems. Some obstacles facing the
therapeutic music design process like technological awareness, cultural
sensitivity, therapeutic music design protocols, and standardization of
therapeutic protocols are also discussed. The results indicate that the
combination of modern technologies and music therapy procedures can greatly
increase the opportunities of sound-based medicine in healthcare. The future
of research is in creation of AI-controlled individualized music therapy
systems, immersive therapeutic spaces, and standardized clinical models that
will enable the further integration of music therapy into the modern
healthcare systems. |
|||
|
Received 19 January 2026 Accepted 25 March
2026 Published 03 April 2026 Corresponding Author Nisha
Wankhade, nisha.wankhade@gmail.com DOI 10.29121/shodhkosh.v7.i3s.2026.7446 Funding: This research
received no specific grant from any funding agency in the public, commercial,
or not-for-profit sectors. Copyright: © 2026 The
Author(s). This work is licensed under a Creative Commons
Attribution 4.0 International License. With the
license CC-BY, authors retain the copyright, allowing anyone to download,
reuse, re-print, modify, distribute, and/or copy their contribution. The work
must be properly attributed to its author.
|
|||
|
Keywords: Music Therapy, Sound Healing, Healthcare Technology,
Digital Health Systems, Artificial Intelligence, Wearable Sensors,
Neurological Rehabilitation, Immersive Therapeutic Environments |
|||
1. INTRODUCTION
1.1. Background of Music Therapy in Healthcare
Music therapy has become a significant adjunctive method in contemporary medicine combining artistic expression and clinical treatment to help in the physical, emotional, and psychological welfare. The therapeutic application of music is of ancient origin and evidence of sound and rhythm-related healing practices has been observed in ancient societies worldwide. Music therapy is becoming increasingly accepted as a formal therapeutic intervention in modern healthcare systems provided by trained professionals to achieve better patient outcome. Hospitals, rehabilitation centers, and mental health institutions have started to implement music therapy in the treatment program of patients with stress, anxiety, neurological illnesses and chronic pain. Neuroscience and psychology research has shown that the musical stimuli may have an effect on brain activity, mood, and other physiological reactions like heart rate and blood pressure. This has led to the emergence of music therapy as an important non-pharmacological intervention complementing the traditional medical interventions and ensuring holistic care of the patients De Witte et al. (2022).
1.2. Role of Sound and Therapeutic Music in Healing
Sound and music are important in controlling emotional and physiological functions of the human body. Rhythm, melody, harmony and tempo are musical elements capable of stimulating the memory, emotional and motor control parts of the brain. Therapeutic music interventions are typically the activities where the listeners listen to specially chosen pieces, actively play music, or passively experienced the sound with the aim of inducing relaxation and emotional expression. Indicatively, a slow rhythmic music can lessen stress and anxiety by decreasing the level of cortisol and enhancing the breathing patterns. In the same manner, rhythmic auditory stimulation has been applied in neurological rehabilitation to enhance motor coordination in patients who have suffered a stroke or in patients with Parkinsonism. Music will also enable communication of feelings and give the patient a non-verbal avenue of communicating his feelings that might be hard to communicate. All of these mechanisms allow sound-based treatments to provide greater psychological resilience, decrease perception of pain, and overall well-being of a patient.
1.3. Emergence of Digital Technologies in Music Therapy
The recent developments in technology have greatly increased the opportunities of providing music therapy within a healthcare context. Therapeutic environments are getting integrated with digital audio technologies, mobile health applications, wearable sensors and artificial intelligence systems. These technologies make it possible to form individualized music therapy programs, which can depend on the needs of patients and their physiological reactions. As an example, biological indicators like heart rate variability and stress level can be tracked by wearable devices and used to dynamically change the soundscapes in real-time by the music therapy systems. The increased accessibility of music therapy has been facilitated by mobile applications and online platforms that allow a therapist to receive a therapy session remotely and also allow home-based therapy to be conducted. Moreover, multisensory therapeutic environments, including virtual reality (VR) and augmented reality (AR) technologies, are also being considered to ensure that the visual and auditory stimuli are incorporated to ensure the patient is more engaged. Technological inclusion is thus a revolutionary move in the development of musical therapy practices.
1.4. Research Problem and Motivation
Although there is an increasing popularity of music therapy and its proven effectiveness, certain obstacles still persist regarding the successful introduction of sound-based forms of therapy to the contemporary healthcare technologies. Several of the currently existing music therapy practices are based on conventional approaches that might be insufficiently scalable, personal, and with an analytical approach. Moreover, healthcare facilities usually do not have a well-organized technological infrastructure that would enable the combination of the therapeutic sound intervention with the patient monitoring system and digital health technology. The lack of standard models on technology-enabled music therapy narrows its wider application to clinical settings. These challenges have inspired the need to investigate the way in which upcoming technologies can make the process of music therapy interventions more effective, more readily available, and more personalized. To close the gap between the past and the present healthcare systems, it can be recommended to develop integrated frameworks, incorporating the principles of sound therapy with the use of digital technologies Grau-Sánchez et al. (2022).
1.5. Objectives of the Study
The main aim of the present work is to explore the overlap between sound, technology, and the field of healthcare as per the context of music therapy. Precisely, the study is seeking to analyze how technological advancements can be utilized and help boost therapeutic music interventions in clinical settings. The study is also aimed at surveying the existing literature on the topic of music therapy application, examining the use of digital technologies in the delivery of therapeutic sounds, and determining the current issues related to the implementation of music therapy systems in healthcare facilities. Moreover, the study suggests a conceptual model of an integrated technology-based music therapy model that aids in offering customized therapeutic experience and evidence-based assessment of patient outcomes. Exploring these aspects, the study will serve to develop a better and more accessible approach to music therapy.
2. Background and Foundations of Music Therapy
2.1. Historical Development of Music Therapy
The history of music therapy is long-established based on the perception of the therapeutic nature of sound and music. Music was employed in the spiritual rituals, meditation, and healing of people in ancient Greek, Egyptian, Indian, and Chinese civilizations. Philosophers and scholars in ancient Greece, like Pythagoras and Plato, held that music harmony could modify the feelings of man and re-establish harmony in the body and mind. Equally, the Indian traditional healing systems had sound vibrations and chanting as means of spiritual and psychological health. In the nineteenth and early twentieth centuries, the scientific examination of music and its influence on the human body started being noticed. After both World Wars musicians were playing in hospitals to help recover soldiers who were injured, music therapy became a professional field. Throughout the years, there was the creation of academic programs, research centers and associations to train music therapists and facilitate clinical research in the area.
2.2. Psychological and Neurological Basis of Sound Healing
The music therapeutic effects are directly related to how the human brain perceives sound and rhythm. Neuroscientific research has proven that music stimulates several regions of brain at once such as those involved in emotion, memory, attention, and motor coordination. The brain releases the neurotransmitters, dopamine and serotonin, when people listen to or interact with music and these can be linked to pleasure, motivation, and emotional control. These somatic reactions can be used to explain why music is able to decrease stress, uplift mood, and increase cognitive ability. Also, rhythmic auditory stimulation has been found to have relationships with motor systems within the brain, which are useful with neurological rehabilitation of patients with a movement disorder. Music also has the capacity of arousing autobiographical memory which is particularly useful with people with cognitive impairments like dementia or Alzheimer disease. Sound-based interventions are an effective way to engage with therapy and heal patients through these psychological and neurological processes.
2.3. Types of Music Therapy Approaches
Music therapy practices can be broadly divided into two broad categories, namely active music therapy and receptive music therapy. As active music therapy, the patients are directly involved in the production of music by doing activities like singing, playing musical instruments, writing songs or improvising a rhythm. Such activities promote emotional expression, socialization and cognitive activity. Motor coordination and creativity may also be increased through active participation, especially in the rehabilitation context. Receptive music therapy, in contrast, is based on listening experience in which patients listen to specific music pieces that are chosen to induce relaxation, reflection, or reaction to emotions. During listening to music, therapists can lead patients using imagery or breathing techniques or meditate. There are other therapeutic modalities that combine sound-based programs in a form of rhythmic entraining, vibroacoustic therapy and guided music imagery in addition to these two major approaches. Both methods are individualized to meet the unique needs of the patient and treatment objectives set by the medical practitioners Howlett et al. (2022).
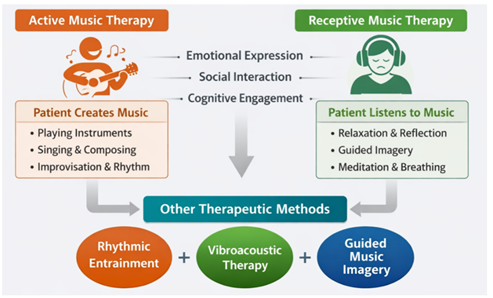
Figure 1
Figure 1 Types of Music Therapy Approaches
The Figure 1 demonstrates the key forms of music therapy techniques applied to the healthcare settings. Active Music Therapy is characterized by the fact that patients actively build music. Patients can sing, play musical instruments, compose song or improvise rhythms. These activities assist patients to release feelings, enhance their socialization, and provoke cognitive processes. The motor coordination and creativeness that is improved by active participation is also useful in rehabilitation and in neurological recovery. Receptive Music Therapy, on the contrary, revolves around therapeutic experiences using listening. In this method, the patients are subjected to listening to apposite music pieces that are meant to encourage relaxation, emotional reflection or mental concentration. Examples of activities that therapists can take patients through include meditation, breathing, or guided imagery with the help of music. The approach is usually employed in stress reduction, emotional control, and relaxation therapy. Besides these two general approaches the diagram also points out other therapeutic techniques which combine sound-based techniques. These are rhythmic entrainment, where the body moves in sync with the musical beats to enhance motor coordination; vibroacoustic therapy, whereby low-frequency sounds vibrations are applied to help patients experience relaxation and alleviate pain; and guided music imagery where patients visualize what they are listening to as they listen to music to aid emotional processing.
2.4. Clinical Applications of Music Therapy in Healthcare
The is a great variety of healthcare facilities where music therapy has been implemented: hospitals, rehabilitation centers, mental clinics, and long-term care facilities. Music therapy has been applied in mental health treatment to minimize the symptoms of anxiety, depression, and trauma by offering the patient a secure and expressive way of communicating emotions. Music based interventions are used in neurological rehabilitation to enhance the motor coordination, speech recovery, and cognitive functioning following a stroke or traumatic brain injury. Another widespread use of music therapy is in pain management and palliative care to bring comfort and emotional support to the patients with chronic illness or terminal conditions. Music therapy can be applied in the work of a pediatric setting of healthcare facilities to decrease stress and fear related to medical procedures among young patients. Equally, in geriatrics, music therapy is capable of triggering memory and enhancing the quality of life of elderly individuals with mental deterioration. The above clinical applications underscore the multiracial nature of music therapy as a supportive therapeutic intervention in any healthcare system.
2.5. Benefits of Music Therapy for Physical and Mental Health
Music therapy has got its benefits that are both physical and psychological in the health aspect. On the physiological level, music is able to affect the heart rate, blood pressure, breathing rate and even hormonal level, thus the music can help to control the stress response of the body. Relaxing music has been found to decrease the amount of cortisol in the body, decrease the level of muscle tension and achieve relaxation, which can be useful in stress management and pain relief. In psychological terms, music therapy has the potential to boost emotional expression, mood and enhance coping mechanisms in patients in need of coping with illness or psychological distress. Music also facilitates the process of socializing and communicating, especially in the group therapy where people can work together in music. Moreover, listening to music may enhance the cognitive abilities of people in terms of attention, memory, and problem-solving skills. Since music therapy is the treatment approach that combines emotional, cognitive, and physiological domains of health in a single approach, it is a part of a holistic approach to patient care and well-being Thompson et al. (2023).
3. Literature Review
3.1. Music Therapy in Clinical and Medical Research
There is an increasing amount of clinical and medical research evidence on the therapeutic power of music in a healthcare setting. Many researchers have proven that music therapy is able to influence the psychological state of a patient greatly, as well as aid in physical rehabilitation. In hospitals and rehabilitation centers, clinical trials have revealed that music therapy can lessen anxiety, depression and emotional distress in patients receiving medical care. As an example, studies carried out in oncology care have shown that music therapy is capable of reducing stress related to the treatment and enhancing the emotional strength of patients. Equally, research in the operating rooms has discovered that patients who listen to relaxing music either prior to or after undergoing medical operations tend to have less pain and anxiety. These results indicate that music therapy is a good complementary practice, which improves patient comfort and emotional stability in addition to traditional medical therapies Raglio et al. (2017).
3.2. Sound-Based Therapeutic Interventions
Sound based therapy interventions are not limited to music listening but are categorized into several methods which use sound vibrations and rhythmic stimulation to aid the healing process. Vibroacoustic therapy, rhythmic auditory stimulation and sound meditation are some of the techniques that have been studied in clinical and wellness settings. Vibroacoustic therapy is low frequency sound vibrations which are administered using special equipment to help in relaxation of the muscles and alleviation of pain. Rhythmic auditory stimulation commonly applied in neurological rehabilitation assists patients to enhance motor coordination and gait by coordinating movement of the body to rhythmic sound patterns. Also, sound meditation and therapeutic soundscapes have been applied to assist in reducing stress, mindfulness, and emotional balance. Studies on this topic have indicated that sound environments carefully designed have the potential to affect physiological reactions like heart rate variability and brainwave activities, and hence lead to relaxation and cognitive effect management.
3.3. Technology-Assisted Music Therapy Systems
The new developments in the digital technology have resulted in the creation of technology-aided music therapy systems that are meant to augment therapeutic interventions. Researchers have examined the possibility of using computer-based music systems, mobile applications and digital platforms to provide personalized music therapy experiences. These systems enable therapists to tailor music material according to patient preferences, emotional condition and clinical goals. Moreover, artificial intelligence and machine learning algorithms are also being incorporated into music therapy systems to read patient responses and change therapeutic music on-the-fly. Physiological indicators (heart rate, stress, and sleep) can be monitored by wearable devices with a biometric sensor, which means that therapeutic sound environments can be dynamic. The possibilities of such technological advancements are to enhance the accessibility, scalability, and customization of music therapy practice in remote healthcare environments and in telemedicine services.
Table 1
|
Table 1 Summary of Recent Research in the Domain of Healthcare |
|||
|
Healthcare Focus |
Method |
Key Contributions |
Limitations |
|
Anxiety reduction across
healthcare and clinical settings Wilson (2021) |
Systematic review with
multilevel meta-analysis of 51 studies and 93 effect sizes |
Shows that music therapy has
meaningful anxiety-reducing effects across multiple contexts; also examines
moderators such as intervention design and study factors |
Mixed study designs,
variation in settings and interventions, and exclusion of dementia
populations limit generalizability |
|
Cardiothoracic surgery
recovery Lena et al. (2023) |
Systematic review,
meta-analysis, and trial sequential analysis |
Found reductions in anxiety,
pain, heart rate, systolic blood pressure, and opioid use, with improved
oxygen saturation after surgery |
Evidence is limited to
cardiothoracic surgery patients; protocol heterogeneity may affect
consistency |
|
Dementia care Brancatisano et al. (2020) |
Systematic review and
meta-analysis of 24 RCTs |
Demonstrated improved
cognitive function, lower depression, and lower anxiety in dementia patients;
identified dose-related factors such as session number and duration |
No significant effect on behavior or quality of life; outcomes vary with
intervention length and frequency |
|
ICU anxiety and delirium Golcha et al. (2024) |
Meta-analysis and systematic
review of 14 RCTs |
Reported that music therapy
safely reduced anxiety and supported stability of HR, RR, and SBP in ICU
patients; suggested 15–30 minutes may be optimal |
Effects were weaker or
unclear with longer sessions; limited physiological outcome consistency
across studies |
|
Non-fluent aphasia
rehabilitation Mercier et al. (2024) |
Systematic review and
meta-analysis of RCTs |
Supports neurologic music
therapy for improving repetition ability and speech-related recovery in
aphasia |
Calls for larger samples and
better dose optimization; evidence still narrow for different aphasia
subtypes |
|
Neurologic inpatient
rehabilitation Murtaugh et al. (2024) |
Qualitative study on
development and integration of a music therapy program |
Important for implementation
science; shows how music therapy can be embedded into inpatient
neurorehabilitation services |
Qualitative design does not
establish causal clinical effectiveness; findings may be context-specific |
|
COPD and chronic disease
care Campbell (2020) |
Systematic review and
meta-analysis of 11 studies, 947 patients |
Found benefits for quality
of life and exercise endurance; passive music therapy showed favorable effects on some outcomes |
Effects on dyspnea, anxiety, and depression remain uncertain; more
high-quality RCTs are needed |
Table 1 reveals that this recent literature supports most strongly the use of music therapy in reduction of anxiety, cognitive and emotional outcomes in dementia, perioperative recovery and neurological rehabilitation, particularly in Parkinson’s disease, aphasia and mild cognitive impairment. Implementation studies, biomarker-based evaluation and condition-specific meta-analyses are also increasingly interested in recent work. One of the similar tendencies in these articles is that music therapy has a potential but is constrained by lack of homogeneity in types of interventions, dosage, outcome measures, and quality of studies. It is common in many of these reviews to require larger randomized trials, standardized protocols, increased reporting, and improved combination of physiological and patient-reported outcomes.
3.4. Research Gaps in Technology-Enabled Music Therapy
Although there has been massive strides towards the cognisance of the advantages of music therapy, there are still a number of research gaps in incorporating technology in the sound therapy treatments. Most of the available research centres more on the conventional methods of therapy without necessarily taking time to understand the potential of the new emerging technologies in improving personalization, and data driven treatment methods. Few standardized frameworks to combine music therapy systems and digital health infrastructure, as well as patient monitoring technologies, are also researched. More so, music therapy systems based on artificial intelligence and therapeutic environments based on virtual reality are some of the fields that need to be explored even more. There is also a challenge of ethical issues of privacy of patient data and cultural sensitivity of therapeutic music design. These gaps in research need to be addressed to come up with elaborate and technologically sophisticated models of music therapy that could easily be adopted in the contemporary healthcare systems Altenmüller and Schlaug (2013).
4. Technologies Supporting Music Therapy
4.1. Digital Audio Processing and Therapeutic Sound Design
The digital audio processing technologies are very instrumental in the design and provision of therapeutic music experiences. Sound engineering and other advances in digital signal processing enable therapists and researchers to create personalized soundscapes based on a particular therapeutic outcome. Using computer applications, one can precisely manipulate musical components and elements like tempo, frequency, rhythm, and harmony to have an impact on emotional and physiological reactions. As an example, a slow-tempo music that has soft harmonic configurations is typically employed to make people relax and feel less anxious, whereas rhythmic patterns may trigger the cognitive and motor processes. Sound synthesis platforms and the digital audio workstations allow creation of dedicated therapeutic sound scapes that can incorporate natural sounds, instrumental music and ambiences. The technologies enable the accurate regulation of the sound parameters to make music therapy sessions less spontaneous and responsive to the needs of the patients.
4.2. Wearable Devices and Biometric Sensors
The use of wearable health technologies has established new possibilities of combining music therapy with physiological monitoring systems. Smartwatch, fitness bracelets, biosensors, etc. can also constantly monitor such biometric signals as heart rate, heart rate variability, respiration rate, etc. These physical indicators will be useful in providing information that may be exploited to determine the emotional and physical well-being of the patient in the course of therapy. When wearable sensors are connected to digital music therapy systems, adaptive therapeutic systems that vary music components according to real-time biometric feedback will be possible. To illustrate, in case the stress level of a patient rises, the system will automatically switch to the calming music or slower rhythm patterns to encourage the patient to relax. With this type of biofeedback-oriented music therapy systems, the therapist is able to administer a more customized therapy and also helps the therapists to track the progress of the patient more efficiently Varagani (2026).
4.3. Artificial Intelligence in Personalized Music Therapy
Artificial intelligence (AI) is also recently being considered as a means of improving personal music therapy interventions. With the help of AI algorithms, one can analyze extensive data on musical features and patient reactions and pinpoint the trends that affect the effects of the therapeutic process. Machine learning algorithms can be trained to suggest music choices that reflect the mood, health or other medical condition, or tastes of a patient. Also, AI systems are capable of producing adaptive music pieces, which change dynamically throughout the treatment process. The feedback of patients and physiological responses can also be analyzed with such smart systems to optimize therapeutic playlists and enhance treatment effectiveness in the long term. With the assistance of AI in selecting and analyzing music, the music therapy process can be improved to enable therapists to provide a more effective and more personalized therapeutic intervention.
4.4. Mobile Applications and Digital Music Therapy Platforms
Accessibility of the services of the mobile technology has contributed immensely to the availability of music therapy. Web based systems and mobile applications enable patients to experience therapeutic music programs in non-clinical environments. Guided listening, relaxation, mood tracking software, and playlists of therapeutic music are some of the features that are usually presented in these digital platforms. Certain platforms also facilitate distant communication between therapists and patients, which facilitates music therapy via telehealth. Such flexibility is especially useful with those people who might not have an easy access to face-to-face therapy due to a lack of geographic, physical or economic means. Moreover, music therapy platforms can gather information on user interactions that can be used by researchers to understand how the patients engage in therapy and optimise the design of the therapy program Moreno-Morales et al. (2020).
4.5. Virtual Reality and Immersive Therapeutic Environments
Immersive multimedia and virtual reality (VR) technologies are becoming new in the field of music therapy to improve its experiences. VR settings have the ability to integrate therapeutic music with aesthetically immersive scenery which may be natural environment, relaxing virtual worlds or interactive art scenes. Immersive technologies make it possible to intensify emotional involvement and enhance relaxation by involving several senses at the same time. VR-based music experiences have also been examined in the context of therapeutics on stress management, distraction of pain during medical treatment, and mental health provision. One can guide patients through the virtual environments and listen to the therapeutic soundscapes, which is more engaging and immersive to the healing experience. The therapists can also use these technologies to create custom environments that support certain therapeutic objectives.
4.6. Neurofeedback and Brain–Computer Interfaces
Neurofeedback devices and brain computer interfaces (BCIs) are a new high-tech interface to technology-assisted music therapy. Such systems track the brain activity with the help of electroencephalography (EEG) or some other neural sensing methods and convert brain signals into user feedback. Applied to music therapy, the neurofeedback systems have the ability to vary musical parameters based on the brain activity of the patient so that the musical content rewards being relaxed or focused. As an illustration, the calming music can be made more noticeable when the neural signals of the patient show stress, or increased neural activity. Brain-computer interfaces provide an interface with the musical systems by allowing patients with minimal physical capabilities to use neural signals in communication. These technologies are in the experimental stage, but have a great potential of creating highly personalized therapeutic environments which directly react to the neurological conditions and cognitive functioning. Dhaku Jadhav et al. (2025)
5. Applications of Music Therapy in Healthcare
5.1. Music Therapy for Mental Health and Stress Reduction
Music therapy has emerged as a useful treatment tool to assist in the enhancement of mental health and alleviation of mental stress. Music therapy is a common form of treatment in anxiety disorders, depression and trauma of the emotion. Listening to relaxing music or taking part in some musical event may arouse feelings and give the patient a safe setting to digest the emotions. The ability of music to influence mood and control emotional reactions is due to its ability to activate neural pathways that are linked to reward activities and emotional regulation. Formal music therapy in the therapeutic context can involve listening to music, songwriting, improvisation, and listening to music and relaxation. Such exercises enable one to come up with coping measures that can be used to address stress and emotional difficulties. It has also been found that music therapy is able to lower cortisol levels, normalize breathing, and induce the feeling of relaxation and thus it is highly applicable to patients who are under chronic stress or psychological distress. Karule et al. (2025)
5.2. Neurological Rehabilitation and Cognitive Therapy
Music therapy has shown a lot of positive effects in cognitive therapy and neurological rehabilitation. Neurological patients who have stroke, traumatic brain injury, and Parkinson disease recoveries usually have movement impairments, speech impairments, and memory impairments. Interventions involving music have the ability to activate neuro-pathways that facilitate motor control, cognitive, and language revival. Rhythmic sound stimulation, such as that, is also a popular method of physical rehabilitation, where gait patterns and movement coordination in patients with motor disorders are enhanced. The musical rhythm is an external stimulus of the timing that brings more efficiency in the way the brain organizes the physical movement. Also, music therapy can boost the cognitive abilities of an individual like concentration, memory retention, and solving issues. A frequent use of singing exercises in speech therapy is to help patients recover their speech, especially in patients with aphasia. Music therapy offers a comprehensive method of neurological rehabilitation since it involves more than one brain region at a time. Vasanthan and Nandhini (2014)
5.3. Pain Management and Palliative Care
Music therapy has been popular as a therapeutic aid to pain management and palliative care. Patients with conditions of chronic pain or medical procedures are highly likely to be subjected to pain, anxiety, and emotional distress. The therapeutic music can serve as a distraction method which redirects the mind of the patient towards other sensations other than pain and hence perceived pain diminishes. Guided relaxation and calming music are also prevalent in hospitals as a means of helping patients prior to the surgery and after. Music therapy is significant in the palliative care environment where it aims at enhancing the emotional and psychological welfare of patients with terminal illnesses. Individualized music therapy can be comforting, elicit valuable memories and establish a patient-friendly environment. It is also through music therapy that emotional communication is provided where patients are able to communicate in a non-verbal way about illness, fear or grief. Consequently, music therapy helps in enhancing the quality life of the people who are being provided with long-term or end-of-life care.
5.4. Music Therapy for Pediatric and Geriatric Patients
Music therapy has been specifically found to have positive results when used in the pediatric and geriatric groups of patients. Music therapy in pediatric healthcare facilities assists children to overcome stress and anxiety that comes with the process of hospitalization and medical procedures. Medical settings can be less threatening and more entertaining to young patients through musical games and singing along with interactive sound experiences. Emotional expression, as well as cognitive development in long-term-treatment or rehabilitation children is also supported by music. Music therapy is common in geriatrics to help older adults who are either cognitively declining, demented, or suffer Alzheimer disease. Known songs and music memories may help to recall past experiences and feel better. Music therapy in the elderly care centers can be organized in groups that can help them interact with one another and minimize their feelings of isolation or loneliness. Music therapy improves the psychological and social health of the vulnerable groups of patients through these applications. Rawandale et al. (2024)
5.5. Applications in Chronic Disease and Long-Term Care
Music therapy is slowly finding its way into the therapies of chronically diseased and long term patients with ailments. People with cardiovascular disease, cancer, diabetes, and respiratory issues and conditions tend to be suffering continuous stress, exhaustion, and emotional problems. Through music therapy, these patients can overcome the symptoms through relaxation, mood elevation, and mental resilience. In this case, patients under chemotherapy could be in need of music therapy that will help them decrease anxiety and enhance emotional coping during chemotherapy cycles. Equally, clients undergoing a long term rehabilitation programme can apply exercises that involve music as a means of keeping motivated and alert in the process of healing. Music therapy programs are used in long-term care facilities to provide conducive environments that improve the quality of life and emotional well-being of the patients. When used to treat chronic illness, both physically and psychologically, music therapy is a part of a more holistic and patient-centered care.
6. Proposed Technology-Integrated Music Therapy Model
6.1. Design Principles of the Proposed Model
The suggested music therapy model with the use of technologies is aimed at integrating the principles of therapeutic sound with the latest digital technologies in order to provide improved patient care in the health care setting. A number of important design principles, which confirm effective therapeutic results and technological practicability, guide the model. The first principle is personalization, which is the focus on the music therapy interventions adjusted to the needs of the individual patients, their emotional conditions, and their medical conditions. Different patients can react to musical stimuli, and thus, adaptive systems are required to provide a client with a unique therapeutic soundscape. The second principle is to provide data-driven feedback, according to which physiological and behavioral data obtained about patients are taken to monitor the effectiveness of the therapy and modify musical parameters in real-time. The other significant principle is accessibility, where music therapy services must be available not only in the clinic but also using remote health care systems. Lastly, the model facilitates collaboration with the healthcare systems that would allow therapists, healthcare professionals, and digital monitoring systems to collaborate in the provision of holistic treatment of the patients. Venkata et al. (2025)
6.2. System Architecture for Digital Music Therapy
The design of the proposed model comprises of several interlinked components that collaborate to provide customized music therapy experiences. The system has its root in the patient data acquisition module that gathers physiological and emotional measurements by using wearable sensors and patient input systems. A therapy management module processes these data and analyses conditions of patients and identifies correct therapeutic music interventions. The system also has a music generation and delivery component which selects or produces therapeutic music according to the profile of the patient and therapeutic objectives. Moreover, there is a system of interaction where the patients and therapists can communicate with the system using mobile applications, digital dashboards, or clinical monitoring platforms. One of the data analytics components measures patient reactions and therapy results, which will allow improving therapeutic options continuously.
6.3. Patient Monitoring and Data Collection Layer
The patient monitoring and data collection layer will be involved in the collection of physiological and behavioral data in real time during the sessions of music therapy. Here, wearable devices, biometric sensors, and health monitoring systems are used in this layer to record indicators like heart rate, breathing patterns, levels of stress and emotional changes. The data can be used to understand the physical and psychological condition of the patient under therapy. Through continuous gathering and analysis of such data, the system is capable of assessing the reaction of patients to the various forms of music and sound stimulations. Such information-driven benefits help therapists to better adapt the therapy sessions and monitor the progress of the patient in the long term. Besides that, patient self-reports and mood tracking tools can be included in the data collection process to offer the qualitative feedback which complements the physiological measures. Hazarika et al. (2023)
6.4. Therapeutic Music Generation and Delivery Layer
The generation and delivery layer of therapeutic music is charged with the responsibility of music generation and delivery based on the therapeutic objectives. It is a layer that combines digital audio processing, curated music library and algorithmic music generating systems to compose personal sound worlds. The choice of music may be affected by the tastes of patients, the state of their clinical condition, and the real-time withdrawal of physiological indicators provided by monitoring systems. An adaptive music system can also be present with the adaptive music algorithms altering the tempo, rhythm, or tonal features based on the patient feedback and biometric information. Therapeutic music may be presented in various forms including headphones, hospital sound systems, mobile phones, or even in a virtual world of immersion. This layer will make sure that music therapy is applied in different healthcare settings such as hospitals, rehabilitation centers, home-based care environments, and so on by offering flexible delivery methods.
6.5. Interaction and Feedback Mechanisms
A good music therapy presupposes the significant interaction of patients, therapists, and technological systems. The proposed model provides patients with an opportunity to actively engage in their therapeutic experience owing to the interaction and feedback mechanisms involved in the model. The patients can engage with the system via mobile applications, touch interfaces or wearable devices that enable them to choose their music preference, control the intensity of their therapy or even give them a response of their feelings. Digital dashboards also allow therapists to track the response of the patients and adjust the therapy parameters. The system can be included with visual feedback, relaxation instructions or interactive music activities that allow patients to be engaged. The feedback obtained through interaction with patients, as well as physiological measurements, is seen in real-time and enables the system to adjust therapeutic interventions dynamically to ensure a more responsive and personalised healing environment.
6.6. Integration with Healthcare Systems
In order to effectively be used in the clinical setting, the music therapy technologies need to be integrated with the existing healthcare systems. The suggested model will have interfaces that enable the music therapy platform to interface with hospitals information systems, electronic health record, and digital health monitoring platforms. Such integration will allow healthcare practitioners to receive therapy information, track patient progress, and integrate the results of music therapy into general treatment. Also, a safe data management policy will guarantee that the information concerning patients is processed in accordance with healthcare privacy laws. The model encourages the interdisciplinary cooperation between music therapists, physicians, psychologists, and healthcare administrators through combining therapeutic sound systems with healthcare infrastructure. This kind of integration contributes to improving the role of music therapy as a supplementary part of patient-centered healthcare.
7. Evaluation Framework and Performance Metrics
7.1. Clinical Effectiveness Indicators
To measure the success of music therapy in healthcare, the assessment of the program must be conducted through measurable clinical indicators that can be assessed based on the patient health and well-being. Some clinical effectiveness measures can be evaluated by a decrease in anxiety levels, elevation of mood, decrease in pain, and cognitive functioning. Medical observation record, psychological scales, stress assessment questionnaires, and stress assessment scales are some of the standardized assessment instruments used by healthcare professionals to measure these outcomes. Secondly, clinical assessments can focus on analyzing the changes in the quality of sleep, the emotional stability, and the general satisfaction of the therapy sessions in the patients. The ability to track these indicators enables the researchers and healthcare professionals to ascertain whether music therapy interventions are creating a feasible therapeutic effects to the patients in various clinical contexts.
7.2. Patient Engagement and Emotional Response
The involvement of the patients is a critical factor when it comes to the effectiveness of the music therapy interventions. Interested patients will be more participative in the therapy sessions by expressing emotions, and responding to the therapeutic music experiences in a positive manner. Engagement could be assessed by observing the patient engagement rates in the course of music therapy and in the case of digital-based therapies, by digital interaction levels and by self-reported feedback on the emotional state response. The use of emotional responses like relaxation, happiness, emotional release, or alleviated stress can be used as important sources of information on how successful the therapy is. The system of digital music therapy can also monitor engagement based on such metrics as session length, number of sessions, and exposure to therapeutic material. These signs assist therapists in knowing how to relate with music therapy and what will be beneficial to enhance the therapeutic experience by patients.
7.3. Physiological and Cognitive Outcome Measures
Physiological and cognitive outcome measures are used to offer objective data which justify the evaluation of music therapy intervention. The body response to therapeutic music could be reflected in physiological measures like the heart rate, heart rate variability, the blood pressure and cortisol. These measurements can be measured during and after the therapy sessions in wearable sensors and health monitoring devices. These cognitive effects may be an increase in memory, attention, speech recovery, and problem-solving skills especially in patients who have undergone neurological rehabilitation. It is through the examination of these physiological and cognitive indicators that the healthcare providers will be in a better position to know how music therapy affects the physical and mental well-being of the patient. These measurements can also be used in development of evidence based practices in the therapy.
7.4. Usability and Accessibility of Therapy Platforms
In TAM systems of technology-based music therapy, usability and accessibility are significant evaluation measures. The success of online treatment sites is determined by the ease with which patients and healthcare practitioners can use the system. An assessment can be conducted by examining the user interface design, system responsiveness as well as the general ease of use of patients who have different degrees of familiarity with technology. Such aspects as compatibility with assistive technology, multilingual interface, and the ability to work with various devices, e.g. smartphones, tablets and clinical workstations are covered by the accessibility considerations. The surveys of user feedback and usability testing may be helpful to learn more about the way patients and therapists rate the digital music therapy platform. High usability and accessibility are the key to ensuring the prevalence of music therapy technologies in healthcare settings.
7.5. Ethical and Cultural Considerations
Evaluation of music therapy interventions requires ethical and cultural considerations to be important elements. The music used in therapy must be sensitive and culturally aware of the background, beliefs as well as personal preferences of the patients. Relevance to cultures in music choice can be of great importance to patient comfort and emotional involvement. Ethical analysis also entails the preservation of the privacy of patient and maintenance of privacy of personal health information gathered using digital therapy systems. When gathering physiological or behavioral data in the course of therapy, they should be informed. Also, health practitioners should guarantee the responsible use of technological systems in the clinical setting and the presentation of music therapy interventions by qualified professionals. The complexity of such ethical and cultural factors is to be addressed and help to shape responsible and patient-centered music therapy practices.
8. Future Research Directions
8.1. AI-Driven Personalized Music Therapy
With the opportunities that artificial intelligence offers, the future of music therapy can change greatly as it allows offering highly personalized therapeutic interventions. Further studies can be conducted in the field of the creation of intelligent systems that process the information of the patient, his/her emotional experiences, and physiological indicators to suggest or create therapeutic music in real time. Machine learning algorithms might be developed to find patterns in patient responses to various aspects of music like rhythm, tempo, and melody. The AI systems may dynamically control the musical pieces based on biometric parameters such as heart rate, stress levels and brain activity with the aim of enhancing therapeutic outcomes. Furthermore, the generative AI tools can be utilized in generating adaptable soundscapes that reflect the user preferences and clinical needs. More studies should be conducted to determine the effectiveness of AI-assisted music therapy systems, their reliability and clinical safety in a real-world healthcare setting.
8.2. Integration with Smart Healthcare Systems
Digital healthcare infrastructure is now introducing new prospects of combining music therapy with smart healthcare systems. The future research can be based on the creation of interoperable platforms that can be used to integrate music therapy applications into electronic health records, hospital monitoring systems, and telemedicine platforms. This integration would enable medical practitioners to follow up on the progress of patients, observation of treatment results, and integrate music therapy data to larger treatment regimes. The Internet of Things (IoT)-based healthcare systems might be used to monitor patient physiological status in real-time with the help of wearable devices and sensors. Such systems might automatically activate therapeutic music interventions via the detection of signs of stress, anxiety and pain. The research in this field should also cover the issues of data security, system integration, and interoperability of the clinical workflow to make sure that the music therapy technologies can work well in the healthcare ecosystems.
8.3. Multisensory and Immersive Therapeutic Environments
The latest types of immersive computing include virtual reality (VR), augmented reality (AR), and mixed reality (MR) that could be used to develop multisensory therapeutic spaces. The next-generation studies can investigate whether the use of music therapy along with the immersive visual and spatial experience could be effective regarding the emotional involvement and therapeutic effect. As an illustration, patients would be put in relaxing virtual spaces like natural scenery or interactive artistic scenes in which therapeutic soundscapes would be synchronized with visual stimulus. These settings can assist patients to enter more profound levels of relaxation, emotional control, and increase mindfulness processes. Immersive technologies can also find their application in the pain management, rehabilitation exercises, and stress reduction therapies. Nevertheless, additional research is required to determine the long-term efficacy, availability and clinical viability of immersive music therapy settings.
9. Conclusion
This paper presented the overlap of sound, technology, and healing and how music therapy can help in enhancing the well-being of patients in various medical settings. By combining the elements of artistic expression, psychological involvement and physiological activity, music therapy is a holistic approach towards mental and physical health support. The discussion in the present paper reveals that music interventions used as therapy can decrease stress, relieve pain, increase emotional expression, and neurological recovery. The advantages above demonstrate the increasing role of music therapy as a supportive therapy in modern healthcare systems. This paper has investigated the theoretical basis and the history of music therapy with focus on the psychological and neurological processes that determine the effectiveness of music therapy. Sound and musical rhythm have an impact on brain activity and emotional control as well as physiological processes and this demonstrates why music-based interventions are gaining popularity in the clinic. More importantly, the paper has also examined some existing research and identified the application of music therapy in fields like treatment of mental health, rehabilitation, palliative care, and long-term support of the patient. The applications show the versatility of the music therapy as a non-invasive and patient-centered form of therapy. The other important area where the research concentrated was the place of emerging technologies in enhancing the capabilities of the music therapy. The development of digital audio processing, wearable sensors, artificial intelligence, and immersive technologies has provided fresh opportunities in providing a personalized therapeutic experience. The systems of technology-assisted music therapy can monitor the reactions of patients in real time and adjust the therapeutic sounding conditions on the basis of the physiological and emotional states. The music therapy model that is proposed in this paper and is integrated with technology shows the way digital health infrastructure may assist in delivering more personalized therapy, monitoring patients, and evaluating the results of the therapy based on the data. Although these are encouraging trends, there are still some issues associated with the large-scale adoption of technology-based music therapy systems. The problems with the accessibility of technology, the ethical handling of patient data, the cultural sensitivity of therapeutic music development, and the necessity of standardized clinical procedures should be addressed. To resolve these issues, it will be necessary to ensure that the utilization of music therapy technologies is responsible and adequately efficient in the context of healthcare settings. The future studies in this field should be focused on finding new technological aspects of making the music therapy therapy more personal, accessible, and effective. The combination of artificial intelligence, smart healthcare systems, and immersive therapeutic environments can play a major role in changing the manner in which music therapy is administered and assessed. Moreover, cross-cultural researches and universal therapeutic systems will contribute to the enhancement of the scientific base of music therapy practices. Through its ability to connect within the areas of music and technology as well as healthcare, music therapy can become more, and more, significant in aiding the patient-centered healing process and overall healthcare outcomes.
CONFLICT OF INTERESTS
None.
ACKNOWLEDGMENTS
None.
REFERENCES
Altenmüller, E., and Schlaug, G. (2013). Neurologic Music Therapy: The Beneficial Effects of Music Making on Neurorehabilitation. Acoustical Science and Technology, 34, 5–12. https://doi.org/10.1250/ast.34.5
Brancatisano, O., Baird, A., and Thompson, W. F. (2020). Why is Music Therapeutic for Neurological Disorders? The Therapeutic Music Capacities Model. Neuroscience and Biobehavioral Reviews, 112, 600–615. https://doi.org/10.1016/j.neubiorev.2020.02.008
Campbell, M., et al. (2020). Synthesis Without Meta-Analysis (SWiM) in Systematic Reviews: Reporting Guideline. BMJ, 368, l6890. https://doi.org/10.1136/bmj.l6890
De Witte, M., Pinho, A. D. S., Stams, G. J., Moonen, X., Bos, A. E., and Van Hooren, S. (2022). Music Therapy for Stress Reduction: A Systematic Review and Meta-Analysis. Health Psychology Review, 16, 134–159. https://doi.org/10.1080/17437199.2020.1846580
Dhaku Jadhav, K., Majumdar, R., Ahmad Khanday, S., Sarvade, N., Musaev, U., and Akhmedov, S. (2025). Mapping Collaborative Governance for Effective Community Engagement in Urban Hygiene Campaigns. Waterlines, 43(1), 34–43. https://doi.org/10.3362/waterlines.v43i1.36
Golcha, R., Khobragade, P., and Talekar, A. (2024). Multimodal Deep Learning for Advanced Health Monitoring: A Comprehensive Approach for Enhanced Precision and Early Disease Detection. In 2024 5th International Conference on Innovative Trends in Information Technology (ICITIIT) ( 1–6). https://doi.org/10.1109/ICITIIT61487.2024.10580622
Grau-Sánchez, J., Jamey, K., Paraskevopoulos, E., Dalla Bella, S., Gold, C., Schlaug, G., Belleville, S., Rodríguez-Fornells, A., Hackney, M. E., and Särkämö, T. (2022). Putting Music to Trial: Consensus on Key Methodological Challenges Investigating Music-Based Rehabilitation. Annals of the New York Academy of Sciences, 1518, 12–24. https://doi.org/10.1111/nyas.14892
Hazarika, I., Alulama, I. A., Matar, H. S., Ibrahim, M. M., and Albannai, H. Y. (2023). An Analytical Study on the Impact of COVID-19 on CSR and Sustainability from UAE Perspective. Journal of Namibian Studies, 33, 1451.
Howlett, J. R., Nelson, L. D., and Stein, M. B. (2022). Mental Health Consequences of Traumatic Brain Injury. Biological Psychiatry, 91, 413–420. https://doi.org/10.1016/j.biopsych.2021.09.024
Karule, K. P., Sapkal, V., Mirajkar, G., Babajanov, M., Tajne, P., Ahire, L. K., and Qushnazarova, U. (2025). Leveraging Transfer Learning Techniques for Automated Tuberculosis Classification on Chest X-Ray. Indian Journal of Tuberculosis, 72, S512–S530. https://doi.org/10.1016/j.ijtb.2025.11.015
Lena, F., Modugno, N., Greco, G., Torre, M., Cesarano, S., Santilli, M., Abdullahi, A., Giovannico, G., and Etoom, M. (2023). Rehabilitation Interventions for Improving Balance in Parkinson’s Disease: A Narrative Review. American Journal of Physical Medicine and Rehabilitation, 102, 270–274. https://doi.org/10.1097/PHM.0000000000002077
Mercier, L. J., Langelier, D. M., Buchanan, J., Robinson, S., and Plamondon, S. (2024). Development and Integration of a Music Therapy Program in the Neurologic Inpatient Setting: A Qualitative Study. Disability and Rehabilitation, 47, 2304–2313. https://doi.org/10.1080/09638288.2024.2393439
Moreno-Morales, C., Calero, R., Moreno-Morales, P., and Pintado, C. (2020). Music Therapy in the Treatment of Dementia: A Systematic Review and Meta-Analysis. Frontiers in Medicine, 7, 160. https://doi.org/10.3389/fmed.2020.00160
Murtaugh, B., Morrissey, A. M., Fager, S., Knight, H. E., Rushing, J., and Weaver, J. (2024). Music, Occupational, Physical, and Speech Therapy Interventions for Patients in Disorders of Consciousness: An Umbrella Review. NeuroRehabilitation, 54, 109–127. https://doi.org/10.3233/NRE-230149
Raglio, A., Zaliani, A., Baiardi, P., Bossi, D., Sguazzin, C., Capodaglio, E., Imbriani, C., Gontero, G., and Imbriani, M. (2017). Active Music Therapy Approach for Stroke Patients in the Post-Acute Rehabilitation. Neurological Sciences, 38, 893–897. https://doi.org/10.1007/s10072-017-2827-7
Rawandale, U. S., Ganorkar, S. R., and Kolte, M. T. (2024). Variable-Bandwidth Noise Filtering Mechanism for the Hearing Aid System. In A. Katti and R. K. Chourasia (Eds.), Advances in Photonics and Electronics ( XX–XX). Springer. https://doi.org/10.1007/978-3-031-68038-0_13
Thompson, N., Iyemere, K., Underwood, B. R., and Odell-Miller, H. (2023). Investigating the Impact of Music Therapy on Two in-Patient Psychiatric Wards for People Living with Dementia: Retrospective Observational Study. BJPsych Open, 9, e42. https://doi.org/10.1192/bjo.2023.20
Varagani, S. H. N. S. (2026). Applications of AI and Quantum Computing in Healthcare. IJRAET, 14(2), 74–85. https://doi.org/10.65521/ijacect.v14i2.1525
Vasanthan, R., and Nandhini, R. (2014). Activities Based Content for Language Teaching at the College Level: An Indian Classroom Perspective. Man in India, 94(4), 987–995.
Venkata, S. B., Ashirova, A., Karwande, V. S., Aruna, T., Kholiyarov, E., and Singh, S. (2025). Towards Accurate Maritime Surveillance: A Hybrid CNN-Transformer Architecture for Ship Detection in SAR Imagery. In Proceedings of the International Conference on Innovations in Intelligent Systems: Advancements in Computing, Communication, and Cybersecurity (ISAC3 2025). https://doi.org/10.1109/ISAC364032.2025.11156808
Wilson, L., et al. (2021). Understanding the Relationship Between Cognitive Performance and Function in Daily Life After Traumatic Brain Injury. Journal of Neurology, Neurosurgery and Psychiatry, 92, 407–417. https://doi.org/10.1136/jnnp-2020-324492
|
|
 This work is licensed under a: Creative Commons Attribution 4.0 International License
This work is licensed under a: Creative Commons Attribution 4.0 International License
© ShodhKosh 2026. All Rights Reserved.