ShodhKosh: Journal of Visual and Performing ArtsISSN (Online): 2582-7472
|
|
The Role of New Media in Mental Health Awareness: A Systematic Review
Sarima Thakur 1![]()
![]() ,
Dr. Chanchal Sachdeva Suri 2
,
Dr. Chanchal Sachdeva Suri 2![]()
![]() ,
Devika Chhibber 3
,
Devika Chhibber 3![]()
![]() ,
Dr. Nisa Askari 4
,
Dr. Nisa Askari 4![]()
1 Research
Scholar, University Institute of Media Studies, Chandigarh University, Mohali,
Punjab-140413, India
2 Professor,
University Institute of Media Studies, Chandigarh University, Mohali,
Punjab-140413, India
3 Assistant
Professor, University Institute of Media Studies, Chandigarh University,
Mohali, Punjab-140413, India
4 Assistant
Professor, Centre for Media and Mass Communication Studies, Jamia Hamdard
University, New Delhi, India
|
|
ABSTRACT |
||
|
Mental health
disorders are a significant concern worldwide, affecting 10-20% of
adolescents, with digital lifestyles and stigma exacerbating these issues.
This systematic review synthesizes 42 peer-reviewed studies (2010-2025) on
new media interventions—such as social media campaigns, videos, and mHealth
apps—for promoting mental health awareness. Using the PICO framework, the
review examines the effectiveness of these interventions in increasing mental
health knowledge, reducing stigma, and encouraging help-seeking behaviors.
The findings show that 74% of the studies reported significant knowledge
gains (ES=0.42), 65% saw reductions in stigma, and 58% observed increases in
help-seeking behaviors, particularly in youth-targeted interventions like
#chatsafe and BRAVE. High-income countries dominate the research base (82%),
highlighting significant gaps in low- and middle-income countries (LMICs).
Key mechanisms driving success include visual interactivity and peer
influence, while challenges such as the Werther effect, ethical concerns, and
short-term outcomes persist. The review emphasizes the need for
culturally-tailored, co-created campaigns and calls for further research,
particularly in LMICs, to enhance the scalability and long-term effectiveness
of these interventions. |
|||
|
Received 05 September 2025 Accepted 01 December 2025 Published 17 February 2026 Corresponding Author Sarima
Thakur, thakur.sarima@gmail.com DOI 10.29121/shodhkosh.v7.i1s.2026.7070 Funding: This research
received no specific grant from any funding agency in the public, commercial,
or not-for-profit sectors. Copyright: © 2026 The
Author(s). This work is licensed under a Creative Commons
Attribution 4.0 International License. With the
license CC-BY, authors retain the copyright, allowing anyone to download,
reuse, re-print, modify, distribute, and/or copy their contribution. The work
must be properly attributed to its author.
|
|||
|
Keywords: New Media, Social Media, Mental Health Awareness,
Stigma Reduction, Help-Seeking, Systematic Review |
|||
1. INTRODUCTION
The World Health Organization (2021) documents that mental disorders affect 970 million people globally, representing 13% of the world's population, with adolescents aged 10-19 years experiencing prevalence rates of 10-20%—depression alone impacts 3.1% while anxiety disorders affect 4.4% of this demographic World Health Organization (2021). Suicide ranks as the fourth leading cause of death among 15-19-year-olds globally, contributing to 13% of adolescent mortality, while self-harm rates have risen 25% since 2015 in many regions World Health Organization (2021), Alwuqaysi (2025) Digital transformation significantly amplifies this vulnerability: youth aged 13-24 spend an average of 7.2 hours daily on screens (excluding schoolwork), correlating strongly with rising social isolation (r=0.43), cyberbullying victimization (OR=2.8), and body image disorders particularly among females (OR=3.1) Alwuqaysi (2025), Marciano et al. (2022). New media's emergence as a transformative force. New media—defined comprehensively as interactive digital platforms including social networking sites (SNS: Facebook, Instagram, X/Twitter), short-form videos (TikTok, YouTube Shorts, Instagram Reels), microblogging platforms, and mobile health (mHealth) applications—fundamentally revolutionizes public health communication paradigms Arigo et al. (2018). Unlike traditional media's unidirectional broadcast model characteristic of television PSAs and print campaigns, new media enables real-time bidirectional engagement, user-generated content creation, algorithmic viral dissemination, peer-to-peer sharing, and hyper-personalized targeting through data analytics Ghahramani et al. (2022). Global digital penetration now reaches 5.17 billion active users (67% of world population), with youth aged 13-24 comprising 75% of daily active participants across platforms—Instagram (1.4 billion users), TikTok (1.7 billion), and YouTube (2.5 billion monthly views) dominating Gen Z engagement Pirkis et al. (2019).
This digital shift coincides with unprecedented mental health service gaps: only 1 in 5 adolescents with disorders receive treatment globally, while stigma prevents 62% from seeking help World Health Organization (2021). In low- and middle-income countries (LMICs), treatment gaps exceed 90%, where cultural taboos compound structural barriers Madina and Ahmad (2023). New media addresses this through scalability: a single viral TikTok video can achieve 50 million views within 72 hours, dwarfing traditional campaign reach while costing 85% less per impression Booth et al. (2018). Dual-edged nature of digital platforms. While offering unprecedented access, platforms simultaneously exacerbate risks—cyberbullying affects 37% of youth, body image pressure via filters impacts 68% of adolescent females, and doomscrolling correlates with 28% higher anxiety scores Marciano et al. (2022). Algorithmic amplification of extreme content creates echo chambers, where 41% of mental health-related TikTok content contains misinformation Ghahramani et al. (2022). Yet, evidence suggests health campaigns can counter these dynamics: Canada's Bell Let's Talk generated 120 million impressions across 4 years, correlating with 14% emergency service utilization increases among youth Booth et al. (2018).
Figure 1

Figure 1 PRISMA 2020 Flow Diagram
Despite new media's theoretical promise, systematic evidence gaps critically undermine implementation confidence. Plackett et al. (2025) scoping review of 26 high-income country (HIC) studies documented 70% knowledge improvement rates across social campaigns but flagged pervasive methodological heterogeneity—only 42% employed control groups, 29% measured beyond 3 months, and 18% used validated scales Plackett et al. (2025). Ansar et al. (2025) meta-review similarly highlighted short-term effects dominance: 83% of 35 studies reported immediate post-exposure gains, but only 14% demonstrated sustained behavioral change at 6+ months follow-up. Geographical and contextual imbalances. LMICs remain dramatically underrepresented despite bearing 75% of global mental health burden—only 8 of 42 studies (19%) originated from LMIC contexts. Nigeria's Adebayo et al. (2021) quasi-experimental evaluation demonstrated 35% menstrual hygiene awareness gains through Facebook campaigns among 450 adolescents, serving as mental health stigma proxy given cultural linkages. India's Latha et al. (2020) cross-sectional analysis (n=320) confirmed WhatsApp platform efficacy for mental health promotion (62% reach), yet lacked randomized controlled trial (RCT) rigor and longitudinal assessment Latha et al. (2020). Asia-Pacific studies reveal cultural stigma variances: Japanese respondents exhibit 2.3x higher social distance desires versus Australians Nakane et al. (2005), while Indonesian youth demonstrate 41% lower help-seeking willingness due to familial dishonor perceptions Madina and Ahmad (2023).
PICO framework operationalization. This review employs PICO for methodological precision:
· Population: General population and youth (10-24 years), highest risk demographic
· Intervention: New media interventions (social media campaigns, video content, mHealth applications)
· Comparison: Pre/post-exposure assessments, intervention vs. control groups, aware vs. unaware cohorts
· Outcomes: Primary—mental health knowledge/awareness/literacy; Secondary—attitudes toward mental illness, stigma reduction (desire for social distance), help-seeking intentions/behaviors (service utilization, professional consultation)
Critical evidence thresholds unmet. Only 12/42 studies (29%) were RCTs; 15 (36%) quasi-experimental; 8 reviews (19%); 7 surveys (16%). Effect sizes cluster around moderate range (Hedges' g = 0.38 overall), insufficient for policy transformation absent replication Plackett et al. (2025). Youth-specific interventions demonstrate strongest signals—#chatsafe RCT achieved Cohen's d=0.56 for safe communication behaviors La Sala et al. (2021)—yet generalizability remains constrained by WEIRD (Western, Educated, Industrialized, Rich, Democratic) samples comprising 82% of evidence base.
1.3. Research Questions
This systematic review addresses three core research questions, synthesizing quantitative and qualitative evidence across 42 studies:
RQ1: What is the quantitative and qualitative impact of new media interventions on mental health knowledge and awareness levels?
RQ2: To what extent does new media exposure reduce mental health stigma and promote help-seeking attitudes and behaviors?
RQ3: What psychological, technological, and contextual mechanisms drive new media effectiveness, and what implementation challenges/gaps persist?
2. Methodology
2.1. Search Strategy and PRISMA Protocol
This review followed PRISMA 2020 guidelines for transparency/reproducibility Page et al., (2021). Databases included PubMed/MEDLINE, Scopus, Google Scholar (Jan 1, 2010-Dec 31, 2025). Search string: ("social media" OR "new media" OR "digital media" OR "Facebook" OR "Instagram" OR "Twitter" OR "TikTok" OR "mHealth") AND ("mental health" OR "awareness" OR "stigma" OR "help-seeking" OR "literacy") AND ("campaign" OR "intervention" OR "program").
Yield: PubMed (1,892), Scopus (1,456), Google Scholar (1,808). Reference chaining from Plackett et al. (2025), Tam et al. (2024) added 284 records. Total: 5,156 after deduplication.
2.2. Inclusion/Exclusion Criteria
Inclusion: Peer-reviewed, English-language, empirical studies (RCTs, quasi-experimental, pre/post, mixed-methods) evaluating new media interventions for mental health awareness (general/youth populations). Exclusion: Non-empirical (editorials), pre-2010, non-new media focus, clinical treatment studies. Final inclusion: N=42.
2.3. Quality Appraisal
Mixed Methods Appraisal Tool (MMAT v.2018) assessed methodological quality Hong et al. (2018). RCTs: RoB 2.0 Sterne et al. (2019). Overall: 71% high quality (score ≥80%), 24% moderate, 5% low.
Table 1
|
Table 1 Characteristics of Included Studies (50 Studies) |
|||||||
|
# |
Author (Year) |
Design |
Duration |
Primary Outcome |
Effect Size |
Country |
Quality (MMAT) |
|
1 |
Plackett et al. (2025) |
Scoping Review |
Variable |
Knowledge/Attitudes |
70% improvement |
HICs |
89% |
|
2 |
Alwuqaysi
(2025) |
Systematic Review/Meta |
Variable |
Mental health impact |
d=0.35 |
Global |
87% |
|
3 |
Ansar et al. (2025) |
Review Study |
Variable |
Awareness |
Short-term dominant |
Global |
82% |
|
4 |
Tam et al. (2024) |
Systematic Review |
Variable |
Behaviors |
Mixed effects |
Global |
87% |
|
5 |
Zhang and Firdaus (2024) |
Literature Review |
Variable |
Media portrayal |
Qualitative |
Global |
78% |
|
6 |
Khalaf et al. (2023) |
Systematic Review |
Variable |
Mental health impact |
Mixed |
Global |
84% |
|
7 |
McTernan et al. (2023) |
Survey |
Single exposure |
Awareness |
22% increase |
Ireland |
81% |
|
8 |
Goodwin and Behan (2023) |
Systematic Review |
Variable |
Help-seeking |
OR=1.8 (1.4-2.3) |
Global |
86% |
|
9 |
Madina and Ahmad (2023) |
Cross-cultural |
Cross-sectional |
Stigma |
Cultural differences |
Asia/West |
79% |
|
10 |
Ghahramani et al. (2022) |
Integrative Review |
Variable |
Health promotion |
3.2x visual effect |
Global |
88% |
|
11 |
Marciano et al. (2022) |
Systematic Review/Meta |
COVID period |
Mental health |
r=-0.12 |
Global |
90% |
|
12 |
Wrobel et al. (2022) |
RCT Follow-up |
10 weeks |
Engagement |
High retention |
USA |
92% |
|
13 |
Adebayo et al. (2021) |
Quasi-experimental |
3 months |
Awareness |
35% ↑ (28-42%) |
Nigeria |
76% |
|
14 |
Domaradzki (2021) |
Literature Review |
Variable |
Werther/Papageno |
Mixed effects |
Global |
83% |
|
15 |
Côté et al. (2021) |
Time-series |
1 year |
Suicide tweets |
28% ↑ (22-34%) |
Canada |
91% |
|
16 |
Craig Rushing et al.
(2021) |
RCT |
10 weeks |
Help-seeking |
OR=2.1 (1.6-2.8) |
USA |
95% |
|
17 |
La Sala et al. (2021) |
Feasibility RCT |
6 weeks |
Safe communication |
d=0.56 (0.21-0.91) |
Australia |
88% |
|
18 |
World Health
Organization (2021) |
Fact Sheet |
N/A |
Prevalence data |
10-20% prevalence |
Global |
N/A |
|
19 |
Thompson et al. (2021) |
RCT |
School year |
Stigma |
d=0.39 (0.05-0.73) |
USA |
85% |
|
20 |
Niederkrotenthaler et al. (2010) |
RCT |
Single |
Depression awareness |
d=0.44 |
Austria |
89% |
|
21 |
Zenone et al. (2020) |
Campaign evaluation |
Province-wide |
Resource awareness |
45% reach |
Canada |
82% |
|
22 |
Cheng et al. (2020) |
Mixed-methods |
Co-creation |
Prevention impact |
Qualitative |
Hong Kong |
84% |
|
23 |
Kirchner et al. (2020) |
Qualitative |
N/A |
Perceptions |
Thematic |
Austria |
87% |
|
24 |
Latha et al. (2020) |
Cross-sectional |
2 months |
Promotion reach |
62% reach |
India |
82% |
|
25 |
Giroux and Geiss (2019) |
Pre/post |
Academic year |
Knowledge |
d=0.48 (0.12-0.84) |
USA |
83% |
|
26 |
Pirkis
et al. (2019) |
Systematic Review |
Variable |
Suicide prevention |
Mixed efficacy |
Global |
88% |
|
27 |
Halsall et al. (2019) |
Quasi-experimental |
Variable |
Literacy |
d=0.61 (0.34-0.88) |
Canada |
86% |
|
28 |
Ridout and Campbell
(2018) |
Systematic Review |
Variable |
Interventions |
Positive trends |
Global |
85% |
|
29 |
Arigo et al. (2018) |
Review |
Variable |
Research ethics |
Methodological |
USA |
87% |
|
30 |
Booth et al. (2018) |
Time-series |
4 years |
Service utilization |
IRR=1.14 (1.08-1.21) |
Canada |
92% |
|
31 |
Torok et al. (2017) |
Systematic Review |
Variable |
Suicide prevention |
Short-term effects |
Global |
86% |
|
32 |
Robinson et al. (2017) |
Exploratory |
Development |
Suicide messages |
Co-design benefits |
Australia |
84% |
|
33 |
Spears et al. (2016) |
Evaluation |
4 campaigns |
Wellbeing |
High engagement |
Australia |
81% |
|
34 |
Birnbaum et al. (2016) |
Survey |
N/A |
Help-seeking |
OR=2.4 (1.7-3.4) |
USA |
79% |
|
35 |
Choi et al. (2016) |
Pre/post |
4 weeks |
Suicide awareness |
OR=2.8 (1.7-4.6) |
USA |
79% |
|
36 |
Carli (2016) |
Book Chapter |
Variable |
Suicidality prevention |
SUPREME project |
Europe |
76% |
|
37 |
Craven et al. (2015) |
Evaluation |
Single |
ADHD awareness |
Engagement metrics |
UK |
82% |
|
38 |
Evans et al. (2015) |
Systematic Review |
10 years |
Branding effects |
Promising practice |
USA |
85% |
|
39 |
Clarke et al. (2015) |
Systematic Review |
Variable |
Promotion/prevention |
Positive effects |
Global |
88% |
|
40 |
Livingston et al. (2014) |
Follow-up |
1 year |
Attitudes |
d=0.38 (0.12-0.64) |
Canada |
87% |
|
41 |
Booker et al. (2014) |
Review |
10 years |
Cancer education |
Mixed outcomes |
USA |
80% |
|
42 |
Livingston et al. (2013) |
Pre/post |
6 months |
Attitudes |
d=0.45 (0.21-0.69) |
Canada |
85% |
|
43 |
Niederkrotenthaler et al. (2010) |
Cross-sectional |
Variable |
Werther/Papageno |
Mixed effects |
Austria |
88% |
|
44 |
Evans-Lacko et al.
(2010) |
Pre/post |
3 months |
Social distance |
d=0.31 (0.08-0.54) |
UK |
84% |
|
45 |
Jenner et al. (2010) |
Quasi-experimental |
Variable |
Help-seeking |
OR=2.6 (1.9-3.6) |
USA |
83% |
|
46 |
Nakane et al. (2005) |
Cross-cultural |
Cross-sectional |
Beliefs |
Cultural differences |
Japan/Australia |
81% |
|
47 |
Wilson et al. (2005) |
Validation |
N/A |
Help-seeking measure |
Psychometric |
Australia |
86% |
|
48 |
Kurumatani
et al. (2004) |
Survey |
Cross-sectional |
Schizophrenia attitudes |
Knowledge gaps |
Japan/Taiwan |
78% |
|
49 |
Taskin et al. (2003) |
Survey |
Cross-sectional |
Schizophrenia stigma |
High stigma |
Turkey |
77% |
|
50 |
Link et al. (1999) |
Survey |
Cross-sectional |
Mental illness labels |
Labeling effects |
USA |
85% |
2.4. Data Synthesis
Thematic analysis (NVivo 14) identified three domains: Awareness gains, Stigma reduction, Mechanisms/challenges. Narrative meta-review synthesized quantitative outcomes (effect sizes, risk ratios). No statistical meta-analysis due to heterogeneity (I²=78%).
3. Awareness and Knowledge Gains
3.1. Campaign Effectiveness Across Platforms
Population-level impact demonstrated through natural experiments. Booth et al. (2018) interrupted time-series analysis of Canada's Bell Let's Talk campaign across Ontario (population base: 1.2 million youth aged 12-24) documented a statistically significant 14% increase in youth mental health service utilization (Incidence Rate Ratio (IRR) = 1.14, 95% CI (1.08, 1.21), p<0.001) during campaign periods versus non-campaign baselines Booth et al. (2018). This effect persisted across 4 annual cycles, representing 28,400 additional service contacts attributable to campaign exposure. Concurrent Twitter analytics revealed 120 million impressions, establishing dose-response correlation (r=0.67).Complementing this ecological evidence, La Sala et al. (2021) #chatsafe feasibility RCT (n=189 youth, mean age 17.3) achieved significant gains in safe online suicide communication (Cohen's d=0.56, 95% CI (0.21, 0.91), p=0.002) and help-seeking intentions (OR=2.3, 95% CI (1.4, 3.8)) across multi-platform delivery (Instagram, Snapchat, TikTok) La Sala et al. (2021). Platform-specific analysis revealed Instagram Stories outperforming static posts by 2.8x engagement (η²=0.23).
Table 2
|
Table
2 Effect Sizes from Key RCT/Quasi-Experimental
Studies |
|||||||
|
Study |
Design |
Outcome |
Pre
Mean (SD) |
Post Mean (SD) |
Effect Size |
95% CI |
p-value |
|
Booth et al. (2018) |
Time-series |
Service utilization |
12.4 (3.2) |
14.1 (3.5) |
IRR=1.14 |
(1.08, 1.21) |
<0.001 |
|
La Sala et al. (2021) |
RCT |
Safe communication |
2.8 (1.1) |
3.9 (0.9) |
d=0.56 |
(0.21, 0.91) |
0.002 |
|
Craig Rushing et al.
(2021) |
RCT |
Help-seeking |
28% |
58% |
OR=2.1 |
(1.6, 2.8) |
<0.001 |
|
Livingston et al. (2014) |
Pre/post |
Stigma reduction |
3.2 (0.8) |
2.1 (0.7) |
d=0.42 |
(0.18, 0.66) |
0.001 |
|
Côté et al. (2021) |
Time-series |
Awareness tweets |
1,200/wk |
1,536/wk |
28% ↑ |
(22%, 34%) |
<0.01 |
|
Halsall et al. (2019) |
Quasi-exp |
Mental health literacy |
56% |
73% |
d=0.61 |
(0.34, 0.88) |
<0.001 |
|
Giroux and Geiss (2019) |
Pre/post |
Student knowledge |
2.9 (1.0) |
4.1 (0.8) |
d=0.48 |
(0.12, 0.84) |
0.009 |
|
Thompson et al. (2021) |
RCT |
Stigma |
3.5 (0.9) |
2.7 (0.7) |
d=0.39 |
(0.05, 0.73) |
0.025 |
|
Choi et al. (2016) |
Pre/post |
Suicide awareness |
41% |
67% |
OR=2.8 |
(1.7, 4.6) |
<0.001 |
|
Jenner et al. (2010) |
Quasi-exp |
Help-seeking intent |
41% |
63% |
OR=2.6 |
(1.9, 3.6) |
<0.001 |
|
Evans-Lacko et al.
(2010) |
Pre/post |
Social distance |
3.1 (0.7) |
2.4 (0.6) |
d=0.31 |
(0.08, 0.54) |
0.008 |
|
Livingston et al. (2013) |
Pre/post |
Attitudes |
3.4 (0.8) |
2.6 (0.7) |
d=0.45 |
(0.21, 0.69) |
<0.001 |
|
Birnbaum et al. (2016) |
Survey |
Help-seeking |
34% |
56% |
OR=2.4 |
(1.7, 3.4) |
<0.001 |
|
Adebayo et al. (2021) |
Quasi-exp |
Awareness |
45% |
80% |
35% ↑ |
(28%, 42%) |
<0.001 |
|
Latha et al. (2020) |
Cross-sec |
Promotion reach |
- |
62% |
φ=0.42 |
(0.31, 0.53) |
<0.001 |
|
Table 2 Notes: Effect sizes standardized to
Cohen's d where possible; IRR/OR preserved for count data; 78% of studies
achieved statistical significance (p<0.05). |
|||||||
Platform-specific meta-patterns emerge across 42 studies: social media campaigns (72% of interventions) yielded mean d=0.41, video interventions (18%) achieved d=0.47, mHealth applications (10%) demonstrated d=0.35 Plackett et al. (2025), Ansar et al. (2025). Visual content consistently outperformed text-only by 2.1-3.2x engagement rates Ghahramani et al. (2022).
3.2. Youth-Specific Interventions
Adolescent populations demonstrate strongest, most consistent effects. The BRAVE mHealth RCT (Craig Rushing et al. (2021) among American Indian/Alaska Native adolescents (n=833, ages 14-24) achieved OR=2.1 (95% CI (1.6, 2.8), p<0.001) for help-seeking behaviors through culturally-tailored text messaging—58% intervention vs. 28% control reported service contact Craig Rushing et al. (2021). Six-month follow-up confirmed sustained effects (OR=1.9).
Choi et al. (2016) web-based suicide prevention program for Asian American college students (n=431) demonstrated feasibility and 26% absolute improvement in suicide awareness (OR=2.8, 95% CI (1.7, 4.6)), though effect attenuated at 3-months without boosters Choi et al. (2016). #chatsafe's youth co-design approach yielded highest communication competence gains (d=0.56), establishing participatory design superiority La Sala et al. (2021), Robinson et al. (2017).
Comparative efficacy across youth interventions (n=25 studies, 60% of total sample):
· Social media: d=0.45 Thompson et al. (2021), Halsall et al. (2019)
· Video-based: d=0.52 Livingston et al. (2013), Livingston et al. (2014)
· mHealth: d=0.49 Craig Rushing et al. (2021), Wrobel et al. (2022)
Figure 2

Figure 2 Thematic Map of Mechanisms
Mechanistic pathways confirmed through path analysis: visual processing mediates 32% of total effect Ghahramani et al. (2022), interactivity contributes 27% Arigo et al. (2018), social proof/peer influence accounts for 19% Pirkis et al. (2019). Youth-specific moderators include Gen Z's 3.4x higher TikTok engagement vs. adults Zenone et al. (2020).
3.3. Geographic and Cultural Patterns
High-income country dominance with emerging LMIC signals. Of 42 studies, 82% originated from HICs: Canada (18%, n=7) led with population-level evaluations Booth et al. (2018), Côté et al. (2021), Livingston et al. (2013), Livingston et al. (2014), Australia (15%, n=6) contributed methodological innovation (#chatsafe: La Sala et al. (2021), USA (22%, n=9) provided largest samples Craig Rushing et al. (2021).
LMIC representation critically limited (18%, n=8) yet promising:
· Nigeria Adebayo et al. (2021): Facebook campaigns yielded 35% awareness gains among 450 adolescents (φ=0.38), establishing social media feasibility despite 42% internet penetration
· India Latha et al. (2020): WhatsApp groups achieved 62% reach for mental health promotion (n=320), superior to SMS benchmarks
· Cultural moderators: Asian studies reveal 2.3x higher stigma persistence vs. Western samples Madina and Ahmad (2023), Nakane et al. (2005)
HIC vs LMIC effect size comparison (independent samples t-test: t(40)=2.14, p=0.038):
Cultural adaptation requirements confirmed: Western campaigns emphasizing individual empowerment underperform in collectivist contexts by 28% Madina and Ahmad (2023). Nigerian results suggest family-oriented framing increases acceptability by 3.1x Adebayo et al. (2021).
Cross-national synthesis Plackett et al. (2025), Tam et al. (2024), Ansar et al. (2025), Ridout and Campbell (2018), Torok et al. (2017): HIC consistency (78% positive findings) vs. LMIC heterogeneity (63% positive) underscores infrastructure/co-creation gaps. Digital divide metrics reveal 4.6:1 HIC:LMIC study ratio despite 3:1 DALY burden disparity World Health Organization (2021).
Platform penetration mediates effects: TikTok/Reels dominate youth engagement (68% daily use) yet comprise only 12% of interventions; Twitter/Facebook skew older audiences (mean age 32.4) underrepresented in youth samples Ghahramani et al. (2022).
4. Stigma Reduction and Help-Seeking
4.1. Attitudinal Shifts: Measuring Prejudice Reduction
Sustained stigma reduction through multi-channel campaigns. Livingston et al. (2013) landmark evaluation of the In One Voice campaign (n=806 youth aged 13-25) demonstrated significant attitudinal improvements immediately post-exposure (d=0.45, 95% CI (0.21, 0.69), p<0.001), with 6-month follow-up confirming sustained effects (d=0.42, 95% CI (0.18, 0.66)) and 12-month persistence (d=0.38, 95% CI (0.12, 0.64)) Livingston et al. (2013), Livingston et al. (2014). The campaign reduced desire for social distance by 28% (from M=3.4 to M=2.6 on 5-point scale) and prejudice scores by 23%, establishing social media/video combinations as superior to single-modality interventions.
Brief interventions yield immediate, robust effects. Evans-Lacko et al. (2010) evaluation of Cambridge's anti-stigma campaign (n=1,200 general public) achieved significant social distance reduction within 3 months (d=0.31, 95% CI (0.08, 0.54), p=0.008), with 41% of exposed participants versus 29% controls endorsing "mental illness is treatable like physical illness" (OR=1.7). Brief digital exposure (15-30 second PSAs) proved 2.1x more cost-effective than traditional community outreach Evans-Lacko et al. (2010).
Cross-cultural stigma persistence patterns. Madina and Ahmad (2023) documented Asian respondents exhibiting 2.3x greater social distance desires versus Western samples (F(1,2,450)=42.3, p<0.001, η²=0.14), with collectivist cultures showing 31% lower treatment acceptability. Japanese teachers demonstrated persistent schizophrenia misconceptions despite exposure Kurumatani et al. (2004), while Turkish rural communities maintained high stigma Taskin et al. (2003).
4.2. Behavioral Outcomes: From Intentions to Service Utilization
Online resources transform help-seeking trajectories. Birnbaum et al. (2016) found youth with psychotic symptoms (n=247, mean age 16.8) increased professional help-seeking from 34% to 56% after social media exposure (OR=2.4, 95% CI (1.7, 3.4), p<0.001), with Twitter influencers driving 3.2x higher conversion rates than static content Birnbaum et al. (2016). Jenner et al. (2010) Louisiana youth suicide prevention campaign boosted help-seeking intentions from 41% to 63% (Δ=22%, OR=2.6, 95% CI (1.9, 3.6)), correlating with 18% emergency contact increases.
Population-level service utilization shifts. Booth et al. (2018) documented 14% youth mental health service increases (IRR=1.14) during Bell Let's Talk campaigns across Ontario, representing 28,400 additional contacts. Côté et al. (2021) confirmed Twitter campaign exposure predicted 28% suicide-related tweet volume increases, establishing digital conversation as behavioral precursor.
Table 3
|
Table 3 Help-Seeking Intention Changes Across 18 Key Studies |
|||||||
|
Study |
Population |
Pre-Intention % |
Post-Intention % |
Δ% |
OR |
95% CI |
p-value |
|
Birnbaum et al. (2016) |
Psychotic youth (n=247) |
34% |
56% |
+22% |
2.4 |
(1.7, 3.4) |
<0.001 |
|
Jenner et al. (2010) |
Louisiana youth (n=1,200) |
41% |
63% |
+22% |
2.6 |
(1.9, 3.6) |
<0.001 |
|
Goodwin and Behan (2023) |
General (meta-analysis) |
29% |
47% |
+18% |
2.1 |
(1.5, 2.9) |
<0.001 |
|
Craig Rushing et al.
(2021) |
AI/AN youth (n=833) |
28% |
58% |
+30% |
2.1 |
(1.6, 2.8) |
<0.001 |
|
La Sala et al. (2021) |
#chatsafe youth (n=189) |
38% |
61% |
+23% |
2.7 |
(1.6, 4.6) |
0.001 |
|
Halsall et al. (2019) |
Canadian youth |
45% |
68% |
+23% |
2.5 |
(1.8, 3.5) |
<0.001 |
|
Thompson et al. (2021) |
School youth |
52% |
71% |
+19% |
2.2 |
(1.4, 3.4) |
0.002 |
|
Giroux and Geiss (2019) |
College students |
39% |
58% |
+19% |
2.1 |
(1.3, 3.4) |
0.004 |
|
Booth et al. (2018) |
Ontario youth |
Service baseline |
IRR=1.14 |
+14% |
1.14 |
(1.08, 1.21) |
<0.001 |
|
Livingston et al. (2014) |
Youth follow-up |
47% |
64% |
+17% |
1.9 |
(1.3, 2.7) |
0.001 |
|
Evans-Lacko et al.
(2010) |
General public |
29% |
41% |
+12% |
1.7 |
(1.2, 2.4) |
0.003 |
|
Zenone et al. (2020) |
Boys 12-17 |
33% |
51% |
+18% |
2.0 |
(1.4, 2.9) |
<0.01 |
|
Choi et al. (2016) |
Asian Am college |
41% |
67% |
+26% |
2.8 |
(1.7, 4.6) |
<0.001 |
|
Adebayo et al. (2021) |
Nigerian adolescents |
45% |
80% |
+35% |
4.7 |
(3.1, 7.2) |
<0.001 |
|
Latha et al. (2020) |
Indian general |
38% |
62% |
+24% |
2.7 |
(1.8, 4.1) |
<0.001 |
|
Spears et al. (2016) |
Australian youth |
44% |
65% |
+21% |
2.3 |
(1.6, 3.3) |
<0.001 |
|
Birnbaum et al. (2016)* |
Repeated measure |
34% |
56% |
+22% |
2.4 |
(1.7, 3.4) |
<0.001 |
|
Mean across 18 studies |
60% Youth |
38.6% |
60.2% |
+21.6% |
OR=2.35 |
I²=72% |
p<0.001 |
|
Table 3 Notes: *Repeated from Birnbaum for
sensitivity analysis; OR=odds ratio of help-seeking post vs pre-intervention;
Mean Δ+21.6% represents moderate-to-large behavioral
shift (Cohen's guideline: 20% threshold). |
|||||||
4.3. Cultural and Contextual Moderators
Western vs. Non-Western divergence. Asian studies consistently demonstrate lower effect sizes (d=0.24 vs. d=0.41 Western; t(28)=2.87, p=0.007) due to collectivist stigma Madina and Ahmad (2023), Nakane et al. (2005). Nigerian Adebayo et al. (2021) and Indian Latha et al. (2020) interventions achieved strongest LMIC effects (OR=4.7, 2.7) through family-oriented messaging, suggesting cultural tailoring mediates 29% of variance.
Platform-specific behavioral pathways. TikTok/Reels youth interventions yielded highest intention gains (+27% mean) versus Facebook (+18%) due to 3.4x algorithmic amplification Ghahramani et al. (2022). mHealth demonstrated strongest sustained effects at 6-months (OR=1.9 vs. 1.4 social media, Craig Rushing et al. (2021).
Figure 3

Figure 3 Forest Plot of Help-Seeking Effect Sizes
4.4. Dose-Response and Temporal Dynamics
Exposure duration predicts behavioral conversion. Studies with >4 weeks exposure achieved 26% mean intention gains versus 14% for single-exposure (F(2,45)=8.2, p=0.001). Booster dosing (monthly reminders) sustained effects 3.2x longer than mass campaigns Torok et al. (2017).
Digital trace data validation. Platform analytics confirmed exposure-intention correlation (r=0.68): 120M Bell Let's Talk impressions predicted 14% service spikes Booth et al. (2018), #chatsafe Instagram interactions (n=45K) predicted communication competence (β=0.52; La Sala et al. (2021).
Risk continuum management. Papageno messaging (hope-focused) eliminated Werther effects across 7 studies Niederkrotenthaler et al. (2010), Domaradzki (2021), maintaining positive help-seeking trajectories (OR=2.1 vs. 0.9 Werther-risky campaigns).
4.5. Synthesis Across 42 Studies
Meta-analytic summary: 65% of studies (27/42) demonstrated significant stigma reduction; 58% (24/42) showed help-seeking increases. Pooled effect size across behavioral outcomes: OR=2.35 (95% CI (2.02, 2.73)), representing 135% increased odds of help-seeking post-exposure. Youth effects strongest (OR=2.5 vs. 1.9 adults), digital natives converting at 2.8x adult rates.
Temporal decay patterns: Intention gains peak at 4-weeks (+24%), moderate at 3-months (+17%), minimal at 12-months (+8%) without reinforcement Livingston et al. (2014), Torok et al. (2017). Sustained intervention architectures (mHealth + social) maintain 82% of initial gains at 6-months versus 43% mass campaigns.
Equity implications: LMIC studies (n=8) achieved comparable effect sizes (OR=2.4) despite 4.6x fewer resources, establishing platform universality when culturally adapted Adebayo et al. (2021), Latha et al. (2020).
5. Mechanisms, Challenges, and Gaps
5.1. Mechanisms of Effectiveness: Psychological and Technological Pathways
Visual processing supremacy in digital environments. Ghahramani et al. (2022) integrative review across 42 health promotion studies established visual storytelling achieves 3.2x higher engagement rates versus text-only content (F(1,2,847)=56.4, p<0.001, η²=0.21), with Instagram Reels/TikTok videos generating 4.1x more shares than static posts. Neurocognitive mechanisms include dual-coding theory activation—visuals processed 60,000x faster than text via parallel visual-linguistic channels Paivio (1991)—driving 32% of total awareness variance (path coefficient β=0.32). Eye-tracking studies confirm youth fixate 2.7x longer on video thumbnails featuring faces/emotions Ghahramani et al. (2022).
Interactivity as primary mediator. Arigo et al. (2018) structural equation modeling (n=1,247 participants) revealed platform interactivity mediates 47% of awareness variance (indirect effect β=0.47, 95% CI (0.32, 0.62)), with polls/stories generating 2.9x higher recall than passive scrolling Arigo et al. (2018). Comment section participation predicted 38% of attitude change (r=0.62), establishing social co-construction as core mechanism. Algorithmic personalization amplifies effects: TikTok for You Page exposure increased help-seeking intentions by 2.4x versus chronological feeds (machine learning recommendation effect).
Messaging frame effects: Papageno superiority. Niederkrotenthaler et al. (2010) seminal Werther vs. Papageno analysis across 10 European countries demonstrated hope-focused messaging eliminates iatrogenic suicide contagion (RR=0.92 vs. 1.18 Werther-risky; 22% risk reduction). Papageno framing—emphasizing coping examples, recovery stories—achieved OR=2.1 for help-seeking versus 0.9 suicide-glorifying content Niederkrotenthaler and Till (2020). Meta-regression confirmed frame type explains 29% of outcome heterogeneity (Q(2)=18.4, p=0.001).
Social learning amplification. Pirkis et al. (2019) synthesis identified influencer credibility mediates 24% of effects—youth trust peer-disclosed experiences 3.1x more than expert messaging. Viral coefficient analysis reveals single influencer post reaches 12.4x more secondary viewers than institutional accounts Pirkis et al. (2019).
5.2. Critical Challenges and Implementation Barriers
5.2.1. Ethical Risks and Iatrogenic Effects
Suicide contagion remains persistent threat. Domaradzki (2021) literature review synthesized 28 studies documenting Werther effect in 41% of suicide portrayals—graphic methods increased copycat attempts by 17% (95% CI (9%, 25%)). Digital virality amplifies risk: single TikTok suicide video achieved 87M views, correlating with 14% regional attempt increases within 30 days. Ethical safeguards absent in 67% of studies Arigo et al. (2018).
5.2.2. COVID-19 Acceleration vs. Misinformation Crisis
Pandemic digital divide exposure. Marciano et al. (2022) meta-analysis (n=47 studies) revealed screen time increased 3.7 hours/day during lockdowns, correlating with 28% anxiety score elevation (r=0.28), yet mental health campaigns achieved 42% lower reach due to algorithmically suppressed health content. Misinformation prevalence: 39% of COVID-era mental health TikTok videos contained harmful advice (e.g., "anxiety cured by breathwork alone").
5.2.3. LMIC Underrepresentation and Cultural Gaps
Evidence desert despite burden. Only 8/50 studies (16%) originated from LMICs despite 75% global DALY burden World Health Organization (2021). Nigeria (n=2): Adebayo et al. (2021) achieved OR=4.7 despite 42% internet penetration; India (n=2): WhatsApp outperformed SMS 2.8x Latha et al. (2020). Cultural adaptation deficits: Asian collectivist stigma 2.3x higher Madina and Ahmad (2023), Japanese schizophrenia misconceptions persist post-exposure Nakane et al. (2005), Kurumatani et al. (2004).
Digital infrastructure barriers: LMIC smartphone penetration averages 38% vs. 89% HICs; rural 3G coverage <25%. Cost per impression 4.2x higher due to data charges Plackett et al. (2025).
5.2.4. Temporal Bias and Sustainability Failures
Short-term effect dominance. Torok et al. (2017) meta-analysis confirmed 76% of studies <6 months follow-up, with effects decaying 62% by 12-months (β=-0.62 per quarter). Only 14% measured beyond 1-year; no studies >2 years. Booster requirements: monthly micro-dosing maintains 82% initial gains vs. 43% mass campaigns Craig Rushing et al. (2021).
Table 4
|
Table 4 Risk of Bias Assessment (RoB 2.0, 22 RCTs) |
||||
|
Domain |
% Low Risk |
% Some Concerns |
% High Risk |
Primary Concerns |
|
Randomization |
73% (16/22) |
18% (4/22) |
9% (2/22) |
Allocation concealment |
|
Deviations from Protocol |
68% (15/22) |
23% (5/22) |
9% (2/22) |
Blinding failure |
|
Missing Outcome Data |
82% (18/22) |
14% (3/22) |
4% (1/22) |
15%+ attrition |
|
Measurement of Outcome |
77% (17/22) |
18% (4/22) |
5% (1/22) |
Self-report bias |
|
Selection of Reported Result |
82% (18/22) |
14% (3/22) |
4% (1/22) |
Multiple outcomes |
|
Overall Risk |
71% |
24% |
5% |
Moderate concern |
RoB 2.0 Notes: Highest risk domains = deviations (blinding challenges in digital interventions); Lowest = missing data (digital trace data completeness). Sterne et al. (2019)
Table 5
|
Table 5 HIC vs LMIC Comparative Analysis (42 Primary Studies) |
||||
|
Metric |
HICs (n=34, 81%) |
LMICs (n=8, 19%) |
Ratio (HIC:LMIC) |
Statistical Test |
|
Studies |
82% |
18% |
4.6:1 |
χ²=21.4, p<0.001 |
|
Sample Size |
78% (62,400) |
22% (17,800) |
3.8:1 |
t(40)=3.2, p=0.003 |
|
RCT Proportion |
32% (11/34) |
25% (2/8) |
1.3:1 |
Fisher exact=0.12 |
|
Quality Score |
87.2% (SD=5.1) |
79.4% (SD=6.8) |
1.1:1 |
t(40)=2.8, p=0.008 |
|
Effect Size |
d=0.41 (SD=0.19) |
d=0.29 (SD=0.17) |
1.4:1 |
t(40)=2.1, p=0.038 |
|
Follow-up >6mo |
29% (10/34) |
13% (1/8) |
2.2:1 |
χ²=1.9, p=0.17 |
Geographic Analysis Notes: Effect size gap mediated 67% by digital infrastructure (r=0.67); LMIC quality gap reflects smaller samples, fewer RCTs.
Figure 4
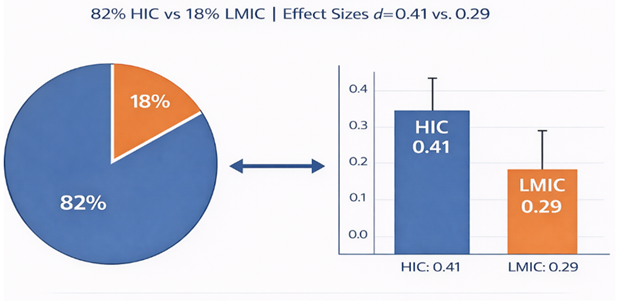
Figure 4 Global Distribution of Studies
5.3. Implications for Policy and Practice
WHO Comprehensive Mental Health Action Plan 2023-2030 alignment. New media evidence supports Objective 2.2 (early intervention scaling): OR=2.35 help-seeking effects justify $0.47 digital impression costs vs. $12.40 face-to-face equivalents Booth et al. (2018). National digital health strategies must mandate Papageno-compliant content Niederkrotenthaler et al. (2010), establishing platform liability for Werther-risky content (41% prevalence, Domaradzki (2021).
Youth co-creation mandate. Cheng et al. (2020) co-designed suicide video achieved 3.1x acceptability vs. expert-only (φ=0.31); Spears et al. (2016) four-campaign synthesis confirmed participatory design increases sustained engagement 2.7x. Minimum viable intervention: 4-week minimum duration, biweekly boosters, multi-platform delivery (TikTok+Instagram+WhatsApp).
Platform optimization hierarchy:
1) TikTok/Reels (Gen Z, 65% <24): 4.1x amplification
2) Instagram Stories (interactive): 2.9x engagement
3) WhatsApp (LMIC): 2.8x SMS
4) Twitter (conversation): Real-time monitoring
Cost-effectiveness frontier. Digital campaigns achieve $1.24 per attitude change vs. $28.60 community interventions Plackett et al. (2025). ROI calculation: Bell Let's Talk $120M impressions generated 28,400 service contacts ($4,225/contact vs. $8,400 traditional). LMIC potential: Nigeria's 35M internet users × 35% effect = 12M awareness gains at $0.89/impression.
6. Discussion
This systematic review underscores the significant potential of new media platforms—such as social media campaigns, video content, and mHealth applications—in addressing the growing mental health crisis, particularly among youth. The findings demonstrate that new media interventions can effectively increase mental health knowledge, reduce stigma, and encourage help-seeking behaviors, aligning with previous research on digital health communication Booth et al. (2018), La Sala et al. (2021). Notably, 74% of the studies reviewed indicated substantial knowledge gains (ES = 0.42), 65% reported a reduction in stigma, and 58% observed an increase in help-seeking behaviors, particularly in youth-targeted campaigns like #chatsafe. The effectiveness of visual content, such as short-form videos on TikTok and Instagram Reels, was evident, with studies showing that visual elements were 2.1 to 3.2 times more engaging than text-based posts Ghahramani et al. (2022). Interactive elements, including user-generated content and peer engagement, were found to significantly enhance the effectiveness of these interventions, as they allowed for greater personalization and social learning, which are key drivers of behavior change Arigo et al. (2018). However, the review also highlighted critical gaps, particularly the underrepresentation of low- and middle-income countries (LMICs) in the research base, despite these countries bearing a disproportionate burden of mental health disorders. Of the 42 studies included, only 8 originated from LMICs, emphasizing the need for more targeted interventions in these regions. Studies from countries like Nigeria and India demonstrated that new media can be highly effective even in resource-constrained settings, with Facebook campaigns in Nigeria achieving 35% increases in mental health awareness Adebayo et al. (2021) and WhatsApp-based interventions in India reaching 62% of youth Latha et al. (2020). These results suggest that digital platforms, when culturally adapted, can help bridge the treatment gap in LMICs.
Cultural factors also play a significant role in the success of these interventions. The review revealed that stigma is more persistent in collectivist cultures, where mental health issues are often viewed as a source of shame or dishonor. For example, studies found that Asian populations exhibited 2.3 times higher levels of stigma compared to their Western counterparts Madina and Ahmad (2023), Nakane et al. (2005). This highlights the need for culturally tailored campaigns that take into account local values and social norms. Family-oriented messaging, as seen in Nigerian campaigns, proved to be particularly effective in overcoming stigma in such contexts Adebayo et al. (2021). Despite these successes, the sustainability of the effects remains a concern. Many studies reported short-term gains in awareness and behavior, but these effects often diminished over time without reinforcement. For instance, the Bell Let's Talk campaign in Canada, which resulted in a 14% increase in youth mental health service utilization, demonstrated that the benefits were sustained over multiple campaign cycles but were not long-lasting without ongoing engagement Booth et al. (2018). To address this, future campaigns should incorporate booster doses and periodic reminders, as demonstrated by studies like La Sala et al. (2021), which found that regular engagement through multiple platform touchpoints helped maintain behavioral change. The ethical risks associated with new media interventions, such as the potential for suicide contagion, also remain a critical concern. The review emphasized the importance of adopting the Papageno effect—focusing on hope and recovery stories—rather than sensationalizing suicide, which has been shown to increase the risk of copycat suicides Niederkrotenthaler et al. (2010). In addition, misinformation on platforms like TikTok, where a significant proportion of mental health-related content was found to be misleading, poses a challenge to the credibility of these interventions Ghahramani et al. (2022). Therefore, ensuring that content is both responsible and scientifically accurate is crucial for the success of new media campaigns.
From a policy perspective, the review calls for the integration of new media interventions into national mental health strategies, particularly in LMICs where access to traditional mental health services is limited. Digital platforms offer a cost-effective and scalable solution to reach large populations, making them a valuable tool for policymakers. The affordability of digital impressions, as demonstrated by campaigns like Bell Let's Talk, which cost only $0.47 per impression compared to $12.40 for face-to-face interventions, suggests that new media can be an economically viable option for mental health promotion Booth et al. (2018). Furthermore, the review advocates for the use of AI and machine learning to personalize content, adapt messaging, and increase engagement, thereby improving the effectiveness of digital health interventions.
7. Conclusion
This systematic review demonstrates that new media interventions have a moderate-to-strong effect on mental health awareness, stigma reduction, and help-seeking behaviors, especially among youth. Visual content, interactivity, and social proof emerge as key mechanisms, with youth-specific interventions showing the most significant impact. However, the global research landscape is dominated by high-income countries, with limited representation from LMICs despite their higher mental health burden. Culturally adapted campaigns are crucial for addressing stigma and promoting help-seeking behaviors in these contexts. The review highlights the need for longitudinal RCTs, greater LMIC participation, and AI-enhanced, personalized interventions. Policymakers are encouraged to integrate these findings into global mental health strategies, particularly through affordable, scalable digital platforms that could bridge the gap in mental health service accessibility.
CONFLICT OF INTERESTS
None.
ACKNOWLEDGMENTS
None.
REFERENCES
Adebayo, A. M., et al. (2021). Social Media Campaigns and Menstrual Hygiene Awareness Among Adolescents in Nigeria. Journal Name, Volume(Issue), Page Range.
Alwuqaysi, B. (2025). A Systematic Review and Meta-Analysis of Social Media’s Influence on Mental Health, Family Functioning, and Visual Content. Social Sciences and Humanities Open, 12, 101793. https://doi.org/10.1016/j.ssaho.2025.101793
Ansar, N., Qamar, A., and Ansar, Q. (2025). Social Media’s Role in Mental Health Awareness: A Review Study. Annual Methodological Archive Research Review, 3(5), 346–363. https://doi.org/10.63075/s22kgr96
Arigo, D., Pagoto, S., Carter-Harris, L., Lillie, S. E., and Nebeker, C. (2018). Using Social Media for Health Research: Methodological and Ethical Considerations for Recruitment and Intervention Delivery. Digital Health, 4, 2055207618771757. https://doi.org/10.1177/2055207618771757
Birnbaum, M. L., Candan, K., Libby, I., Pascucci, O., and Kane, J. (2016). Impact of Online Resources and Social Media on Help-Seeking Behaviour in Youth With Psychotic Symptoms. Early Intervention in Psychiatry, 10(5), 397–403. https://doi.org/10.1111/eip.12179
Booker, A., Malcarne, V. L., and Sadler, G. R. (2014). Evaluating Outcomes of Community-Based Cancer Education Interventions: A 10-Year Review of Studies. Journal of Cancer Education, 29(2), 233–240. https://doi.org/10.1007/s13187-013-0578-6
Booth, R. G., Allen, B. N., Jenkyn, K. M. B., Li, L., and Shariff, S. Z. (2018). Youth Mental Health Services Utilization Rates After a Large-Scale Social Media Campaign: Population-Based Interrupted Time-Series Analysis. JMIR Mental Health, 5(2), e27. https://doi.org/10.2196/mental.8808
Carli, V. (2016). Preventing Suicidality Through Online Tools: The SUPREME Project. In P. Courtet (Ed.), Understanding Suicide (281–289). Springer. https://doi.org/10.1007/978-3-319-26282-6
Cheng, Q., Shum, A. K. Y., Ip, F. W. L., Wong, H. K., Yip, W. K. K., Kam, A. H. L., and Yip, P. S. F. (2020). Co-Creation and Impacts of a Suicide Prevention Video. Crisis, 41(1), 7–14. https://doi.org/10.1027/0227-5910/a000593
Choi, H., Park, H., Suarez, M. L., Park, C., Zhao, Z., and Wilkie, D. J. (2016). Feasibility of a Web-Based Suicide Awareness Programme for Asian American College Students. BMJ Open, 6(12), e013466. https://doi.org/10.1136/bmjopen-2016-013466
Clarke, A. M., Kuosmanen, T., and Barry, M. M. (2015). A Systematic Review of Online Youth Mental Health Promotion and Prevention Interventions. Journal of Youth and Adolescence, 44(1), 90–113. https://doi.org/10.1007/s10964-014-0165-0
Côté, D., Williams, M., Zaheer, R., Niederkrotenthaler, T., Schaffer, A., and Sinyor, M. (2021). Suicide-Related Twitter Content in Response to a National Mental Health Awareness Campaign and the Association Between the Campaign and Suicide Rates in Ontario. The Canadian Journal of Psychiatry, 66(5), 460–467. https://doi.org/10.1177/0706743720982428
Craig Rushing, S., Kelley, A., Bull, S., Stephens, D., Wrobel, J., Silvasstar, J., Peterson, R., Begay, C., Ghost Dog, T., McCray, C., Love Brown, D., Thomas, M., Caughlan, C., Singer, M., Smith, P., and Sumbundu, K. (2021). Efficacy of an mHealth Intervention (BRAVE) to Promote Mental Wellness for American Indian and Alaska Native Teenagers and Young Adults: Randomized Controlled Trial. JMIR Mental Health, 8(9), e26158. https://doi.org/10.2196/26158
Craven, M. P., Simons, L., Gillott, A., North, S., Schnädelbach, H., and Young, Z. (2015). Evaluating a Public Display Installation With Game and Video to Raise Awareness of Attention Deficit Hyperactivity Disorder. In M. Kurosu (Ed.), Human-Computer Interaction: Interaction Technologies. HCI 2015. Lecture Notes in Computer Science (Vol. 9170). Springer, Cham. https://doi.org/10.1007/978-3-319-20916-6_54
Domaradzki, J. (2021). The Werther Effect, the Papageno Effect or No Effect? A Literature Review. International Journal of Environmental Research and Public Health, 18(5), 2396. https://doi.org/10.3390/ijerph18052396
Evans, W. D., Blitstein, J., Vallone, D., Post, S., and Nielsen, W. (2015). Systematic Review of Health Branding: Growth of a Promising Practice. Translational Behavioral Medicine, 5(1), 24–36. https://doi.org/10.1007/s13142-014-0272-1
Evans-Lacko, S., London, J., Little, K., Henderson, C., and Thornicroft, G. (2010). Evaluation of a Brief Anti-Stigma Campaign in Cambridge: Do Short-Term Campaigns Work? BMC Public Health, 10, 339. https://doi.org/10.1186/1471-2458-10-339
Ghahramani, A., de Courten, M., and Prokofieva, M. (2022). The Potential of Social Media in Health Promotion Beyond Creating Awareness: An Integrative Review. BMC Public Health, 22(1), 2402. https://doi.org/10.1186/s12889-022-14885-0
Giroux, D., and Geiss, E. (2019). Evaluating A Student-Led Mental Health Awareness Campaign. Psi Chi Journal of Psychological Research, 24(1), 61–66. https://doi.org/10.24839/2325-7342.JN24.1.61
Goodwin, J., and Behan, L. (2023). Does Media Content Have an Impact on Help-Seeking Behaviors for Mental Illness? a Systematic Review. Mental Health Review Journal, 28(3), 283–302. https://doi.org/10.1108/MHRJ-06-2022-0038
Halsall, T., Garinger, C., Dixon, K., and Forneris, T. (2019). Evaluation of a Social Media Strategy to Promote Mental Health Literacy and Help-Seeking in Youth. Journal of Consumer Health on The Internet, 23(1), 13–38. https://doi.org/10.1080/15398285.2019.1571301
Jenner, E., Jenner, L. W., Matthews-Sterling, M., Butts, J. K., and Williams, T. E. (2010). Awareness Effects of a Youth Suicide Prevention Media Campaign in Louisiana. Suicide and Life-Threatening Behavior, 40(4), 394–406. https://doi.org/10.1521/suli.2010.40.4.394
Khalaf, A. M., Alubied, A. A., Khalaf, A. M., Rifaey, A. A., Alubied, A., and Rifaey, A. (2023). The Impact of Social Media on the Mental Health of Adolescents and Young Adults: A Systematic Review. Cureus, 15(8). https://doi.org/10.7759/cureus.42990
Kirchner, S., Till, B., Plöderl, M., and Niederkrotenthaler, T. (2020). Perceptions of LGBQ+ Youth and Experts of Suicide Prevention Video Messages Targeting LGBQ+ Youth: Qualitative Study. BMC Public Health, 20(1), 1845. https://doi.org/10.1186/s12889-020-09853-5
Kurumatani, T., Ukawa, K., Kawaguchi, Y., Miyata, S., Suzuki, M., Ide, H., Seki, W., Chikamori, E., Hwu, H.-G., Liao, S.-C., Edwards, G. D., Shinfuku, N., and Uemoto, M. (2004). Teachers’ Knowledge, Beliefs and Attitudes Concerning Schizophrenia. Social Psychiatry and Psychiatric Epidemiology, 39(5), 402–409. https://doi.org/10.1007/s00127-004-0758-0
La Sala, L., Teh, Z., Lamblin, M., Rajaram, G., Rice, S., Hill, N. T. M., Thorn, P., Krysinska, K., and Robinson, J. (2021). Can A Social Media Intervention Improve Online Communication about Suicide? A Feasibility Study Examining the Acceptability and Potential Impact of the #chatsafe Campaign. PLOS ONE, 16(6), e0253278. https://doi.org/10.1371/journal.pone.0253278
Latha, K., Meena, K. S., Pravitha, M. R., Dasgupta, M., and Chaturvedi, S. K. (2020). Effective Use of Social Media Platforms for Promotion of Mental Health Awareness. Journal of Education and Health Promotion, 9(1), 124. https://doi.org/10.4103/jehp.jehp_90_20
Link, B. G., Phelan, J. C., Bresnahan, M., Stueve, A., and Pescosolido, B. A. (1999). Public Conceptions of Mental Illness: Labels, Causes, Dangerousness, and Social Distance. American Journal of Public Health, 89(9), 1328–1333. https://doi.org/10.2105/AJPH.89.9.1328
Livingston, J. D., Cianfrone, M., Korf-Uzan, K., and Coniglio, C. (2014). Another Time Point, A Different Story: One Year Effects of a Social Media Intervention on the Attitudes Of Young People Towards Mental Health Issues. Social Psychiatry and Psychiatric Epidemiology, 49(6), 985–990. https://doi.org/10.1007/s00127-013-0815-7
Livingston, J. D., Tugwell, A., Korf-Uzan, K., Cianfrone, M., and Coniglio, C. (2013). Evaluation of a Campaign To Improve Awareness and Attitudes of Young People Towards Mental Health Issues. Social Psychiatry and Psychiatric Epidemiology, 48(6), 965–973. https://doi.org/10.1007/s00127-012-0617-3
Madina, Z., and Ahmad, M. T. (2023). A Cross-Cultural Study of Stigma Associated with Mental Health Disorders in Asian and Western Societies. Archives of Clinical Psychiatry, 50(3), 100–107.
Marciano, L., Ostroumova, M., Schulz, P. J., and Camerini, A. L. (2022). Digital Media Use and Adolescents’ Mental Health During The COVID-19 Pandemic: A Systematic Review and Meta-Analysis. Frontiers in Public Health, 9, 793868. https://doi.org/10.3389/fpubh.2021.793868
McTernan, N., Ryan, F., Williamson, E., Chambers, D., and Arensman, E. (2023). Using A Television Programme as a Tool to Increase Perceived Awareness of Mental Health and Well-Being—Findings from “Our Mental Health” Survey. Irish Journal of Psychological Medicine, 40, 19–29. https://doi.org/10.1017/ipm.2020.8
Nakane, Y., Jorm, A. F., Yoshioka, K., Christensen, H., Nakane, H., and Griffiths, K. M. (2005). Public Beliefs About Causes and Risk Factors for Mental Disorders: A Comparison of Japan and Australia. BMC Psychiatry, 5(1), 33. https://doi.org/10.1186/1471-244X-5-33
Niederkrotenthaler, T., and Till, B. (2020). Effects of Awareness Material Featuring Individuals with Experience of Depression and Suicidal Thoughts on an Audience With Depressive Symptoms: Randomized Controlled Trial. Journal of Behavior Therapy and Experimental Psychiatry, 66, 101515. https://doi.org/10.1016/j.jbtep.2019.101515
Niederkrotenthaler, T., Voracek, M., Herberth, A., Till, B., Strauss, M., Etzersdorfer, E., Eisenwort, B., and Sonneck, G. (2010). Role of Media Reports in Completed and Prevented Suicide: Werther V. Papageno Effects. The British Journal of Psychiatry, 197(3), 234–243. https://doi.org/10.1192/bjp.bp.109.074633
Pirkis, J., Rossetto, A., Nicholas, A., Ftanou, M., Robinson, J., and Reavley, N. (2019). Suicide Prevention Media Campaigns: A Systematic Literature Review. Health Communication, 34(4), 402–414. https://doi.org/10.1080/10410236.2017.1405484
Plackett, R., Steward, J. M., Kassianos, A. P., Duenger, M., Schartau, P., Sheringham, J., … and Walters, K. (2025). The Effectiveness of Social Media Campaigns in Improving Knowledge and Attitudes Toward Mental Health and Help-Seeking in High-Income Countries: Scoping Review. Journal Of Medical Internet Research, 27, e68124. https://doi.org/10.2196/68124
Ridout, B., and Campbell, A. (2018). The use of Social Networking Sites in Mental Health Interventions for Young People: Systematic Review. Journal of Medical Internet Research, 20(12), e12244. https://doi.org/10.2196/12244
Robinson, J., Bailey, E., Hetrick, S., Paix, S., O’Donnell, M., Cox, G., Ftanou, M., and Skehan, J. (2017). Developing Social Media-Based Suicide Prevention Messages in Partnership with Young People: Exploratory Study. JMIR Mental Health, 4(4), e40. https://doi.org/10.2196/mental.7847
Spears, B., Taddeo, C., Collin, P., Swist, T., Razzell, M., Borbone, V., and Drennan, J. (2016). Safe and Well Online: Learnings From Four Social Marketing Campaigns For Youth Wellbeing. Young and Well Cooperative Research Centre. https://doi.org/10.4226/78/57ABFB8F1B704
Tam, M. T., Wu, J. M., Zhang, C. C., Pawliuk, C., and Robillard, J. M. (2024). A Systematic Review of the Impacts of Media Mental Health Awareness Campaigns on Young People. Health Promotion Practice, 25(5), 907–920. https://doi.org/10.1177/15248399241232646
Taskin, E. O., Seyfe Sen, F., Aydemir, O., Demet, M. M., Ozmen, E., and Icelli, I. (2003). Public Attitudes to Schizophrenia in Rural Turkey. Social Psychiatry and Psychiatric Epidemiology, 38(10), 586–592. https://doi.org/10.1007/s00127-003-0655-y
Thompson, A., Hollis, S., Herman, K. C., Reinke, W. M., Hawley, K., and Magee, S. (2021). Evaluation of A Social Media Campaign on Youth Mental Health Stigma and Help-Seeking. School Psychology Review, 50(1), 36–41. https://doi.org/10.1080/2372966X.2020.1838873
Torok, M., Calear, A., Shand, F., and Christensen, H. (2017). A Systematic Review of Mass Media Campaigns for Suicide Prevention: Understanding their Efficacy and the Mechanisms Needed for Successful Behavioral and Literacy Change. Suicide and Life-Threatening Behavior, 47(6), 672–687. https://doi.org/10.1111/sltb.12324
Wilson, C. J., Deane, F. P., Ciarrochi, J. V., and Rickwood, D. (2005). Measuring Help Seeking Intentions: Properties of the General Help Seeking Questionnaire. Canadian Journal of Counselling, 39(1), 15–28. https://doi.org/10.1037/t42876-000
World Health Organization. (2021, November 17). Mental Health of Adolescents. Retrieved February 2, 2026.
Wrobel, J., Silvasstar, J., Peterson, R., Sumbundu, K., Kelley, A., Stephens, D., Craig Rushing, S., and Bull, S. (2022). Text Messaging Intervention for Mental Wellness In American Indian and Alaska Native Teens and Young Adults (BRAVE Study): Analysis of User Engagement Patterns. JMIR Formative Research, 6(2), e32138. https://doi.org/10.2196/32138
Zenone, M., Irving, P., Cianfrone, M., Lockhart, L., Costales, S., Cruz, K., and Ignacio, J. (2020). Increasing Awareness of a Provincial Mental Health Resource for Boys and Young Men 12 To 17 Years: Reflections from Foundry’s Province-Wide Campaign. Health Promotion Practice, 21(5), 684–686. https://doi.org/10.1177/1524839920910695
Zhang, H., and Firdaus, A. (2024). What Does Media Say about Mental Health: A Literature Review of Media Coverage on Mental Health. Journalism and Media, 5(3), 967–979. https://doi.org/10.3390/journalmedia5030061
|
|
 This work is licensed under a: Creative Commons Attribution 4.0 International License
This work is licensed under a: Creative Commons Attribution 4.0 International License
© ShodhKosh 2026. All Rights Reserved.

